Understanding Staph Infections
Staphylococcus aureus, commonly known as “staph,” is a bacterium that can live on a person’s skin. In fact, approximately 20-30% of healthy people are staph carriers. These people are said to be “colonized” by the bacteria, but they are not considered to be ill with an infection. If a colonized person gets a cut on his or her skin, the bacteria can cause skin and soft tissue (ligaments, tendons, fat, and muscle) infections, such as cellulitis, abscesses, impetigo, folliculitis, and furunculosis. People who are not colonized but have a cut or scrape that is exposed to staph can also become infected.
Understanding MRSA and CA-MRSA
Excessive use of penicillin antibiotics over the years has led to the development of stronger strains of bacteria that are no longer killed by penicillin-type antibiotics. Methicillin-resistant Staphylococcus aureus (MRSA) is a strain of staph bacteria that is resistant to penicillin and standard penicillin-related antibiotics. MRSA causes the same types of infections as ordinary staph.
Though MRSA was previously known for being an infection found only in sick people in hospitals, it is now showing up in the general, healthy population. In some regions of the country, MRSA is the most common cause of skin and soft tissue infections. This type of staph infection, known as community-acquired, or community-associated, methicillin-resistant Staphylococcus aureus (CA-MRSA), can be carried by healthy adults and children who do not have any symptoms. Carriers can get a skin or soft tissue infection with CA-MRSA, and non-carriers may get infected from exposure to staph from another person.
MRSA is spread by direct skin-to-skin contact, sharing personal items such as towels, razors, and clothing, and touching surfaces that are contaminated with MRSA. People who are at particular risk of developing MRSA are those who are in close contact with someone with a MRSA infection, have taken antibiotics during the past month, and have a history of a MRSA infection. Not surprisingly, this infection is common in places where people are in close contact, including schools, dormitories, military barracks, correctional facilities, and day-care centers.
Signs and Symptoms of MRSA
It is often difficult at first to tell the difference between an ordinary staph infection and CA-MRSA.
What are some symptoms of a staph skin infection?
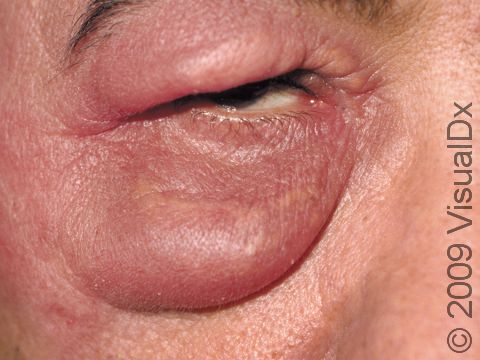
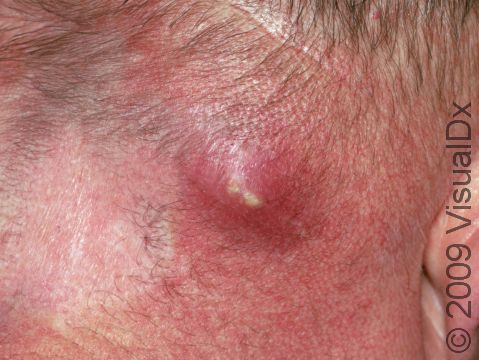
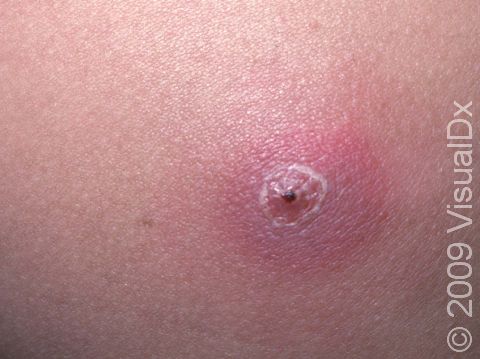
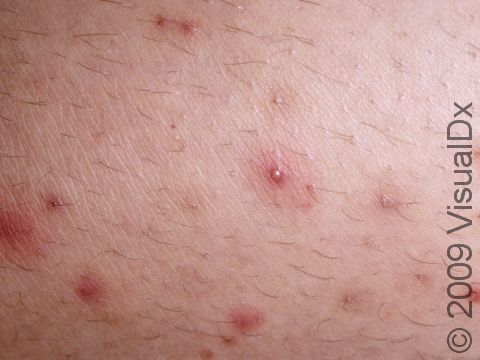
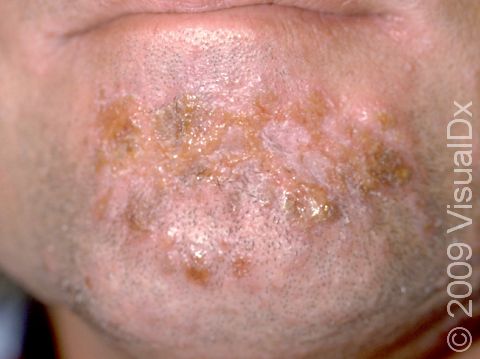
- Red bump that may be pus filled (sometimes mistaken for a spider bite)
- Warmth
- Pain
- Swollen, red, tender skin lesions
If your doctor diagnoses you with a staph infection and you have minimal improvement in your symptoms after a few days, the infection may be a CA-MRSA infection. Signs that you may have a CA-MRSA infection include having the above symptoms coupled with:
- Little to no improvement with antibiotics after 2–3 days
- Rapid spread of the infection
Because CA-MRSA can be passed to others, it is important to follow these prevention tips:
- As a general rule, always maintain good hand-washing habits. This means washing with an antibacterial soap for at least 20 seconds while rubbing your hands together.
- Do not squeeze or attempt to drain any sore.
- Keep any wound covered and clean until it has fully healed.
- Avoid contact with others’ wounds or bandages.
- Do not share personal items such as towels, razors, athletic equipment, sheets, clothes, etc.
- If you or a household member has a wound, wash your laundry in hot, soapy water, with bleach if possible, and dry these items in a hot dryer.
Treatment for MRSA
It is important to note that it is rare for any staph infection to become life threatening in a healthy person. While resistant to penicillin and penicillin-related antibiotics, most CA-MRSA infections can be successfully treated with many other antibiotics. Your doctor may prescribe one or more of the following antibiotics:
- Trimethoprim-sulfamethoxazole (Bactrim®, Septra®)
- Clindamycin (Cleocin®)
- Tetracyclines (such as doxycycline)
- Amoxicillin
- Linezolid (Zyvox®)
It is important to finish all of the antibiotics, even if the infection appears to be healed. In some cases, especially if antibiotics are not working, your doctor may swab the wound to obtain a culture. This helps to specifically identify the bacteria and choose the correct antibiotics.
Your doctor may also drain the infection if there is pus under the skin. This is essential so that the infection can completely heal.
References
Centers for Disease Control and Prevention. Methicillin-resistant Staphylococcus aureus (MRSA): General Information About MRSA in the Community. http://www.cdc.gov/mrsa/community/index.html. Updated March 25, 2016. Accessed November 28, 2016.
Rehm SJ. Staphylococcus aureus: the new adventure of a legendary pathogen. Cleve Clin J Med. 2008;75(3):177-180, 183-186, 190-192. PMID: 18383927.
If you’re a doctor or health care professional, click here for more information.
To learn more about some of the conditions related to staph infection and potential CA-MRSA infection, click any of the images below.
Loren Miller, MD, MPH
Infectious Disease Editor
Associate Professor of Medicine
David Geffen School of Medicine at UCLA
Harbor-UCLA Medical Center