You have probably been hearing a lot about clinical trials recently, especially with regards to the COVID-19 vaccines. While some clinical trials test effectiveness of vaccines for viruses such as COVID-19, countless others study the efficacy of new treatments for all types of diseases, including dermatological conditions. So, what should you do if your dermatologist recommends you for a clinical trial for your skin condition? Here is some information on what clinical trials are, how to find one to participate in, and how you can prepare yourself for the experience, if you choose.
What are clinical trials used for?
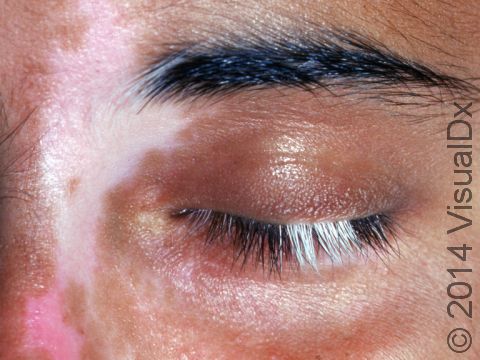
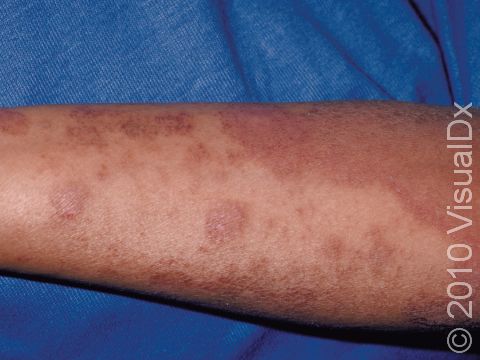
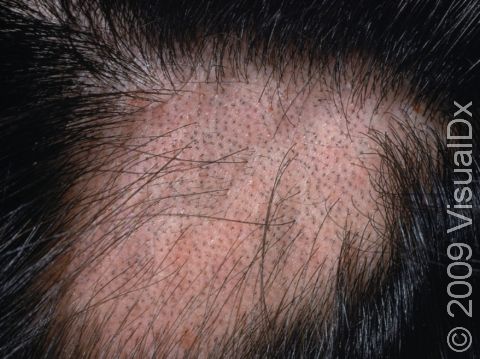
Clinical trials, according to the National Institutes of Health (NIH), are studies where a new intervention—such as a medication—is tested to treat a disease. Patients enroll in clinical trials for a variety of reasons: some diseases still have no treatment approved by the Food and Drug Administration, like alopecia areata or vitiligo, and some patients have severe enough disease that no other medication has helped them. Only after clinical trial testing did dupilumab, for example, become the first injectable medication approved for the treatment of moderate-to-severe eczema.
Where can I find more information about available clinical trials?
Clinicaltrials.gov is the gold standard for finding out more information about clinical trials that are currently available. Your dermatologist may recommend specific studies; but if you’d prefer to do your own digging, the website allows you to filter trials by disease, phase of the trial, enrollment status, and geographic region.
Once you find a specific trial for your disease, the “phase” will be one of the most pertinent pieces of information. A trial in a later phase (up to phase 3), means more patients have already taken the drug—which gives you more information about the drug’s effectiveness and side effects. However, it’s in these later phases that some patients may get the “placebo,” or a non-therapeutic treatment that allows researchers to directly compare the drug’s effectiveness to someone receiving no treatment at all. It’s important to weigh what you value most before enrolling in the trial.
Other useful information includes the “inclusion and exclusion criteria,” which essentially tell you if you are a good candidate for the trial. Some trials, for example, do not allow pregnant patients or those under a certain age to enroll. Once you have decided on a trial, you can always connect with the trial’s site contact, as well as your dermatologist, to find out more information.
If I choose to participate, what can I expect during the clinical trial?
Once you and the site staff have touched base and agreed on a date, you can prepare for your first visit. Since clinical trials are quite thorough, some of the initial visits can take a longer time while you and the site staff get to know one another. This can be mitigated by coming prepared with your medical history, including:
- What medical conditions you have.
- Names and dosages of current medications you’re taking.
- Names of prior medications you have tried for your disease.
Before enrolling you, sites will always provide you with an “informed consent” document that summarizes the study, the risks and benefits of the drug, and your rights as a study participant. It is important to understand that you always have the option of leaving the study.
If you do decide to enroll, then kudos! Clinical trials are exciting opportunities to treat your disease while contributing to new research. While you are enrolled in the study, be sure to let study staff know about changes to your health since the last visit. Clinical trials test new drugs, and patient safety is of the utmost importance—don’t be afraid to let your site know if you have any updates, questions, or concerns.
Last modified on July 6th, 2023 at 10:24 pm