Hair Loss: Understanding Causes & Getting Help from a Dermatologist
Early diagnosis of hair loss is crucial because certain types of hair loss in the category of cicatricial alopecia can result in irreversible damage. To make full use of each dermatology visit, patients can help by being equipped with a basic knowledge on hair loss and an understanding of the goals of your dermatologist during the visit.
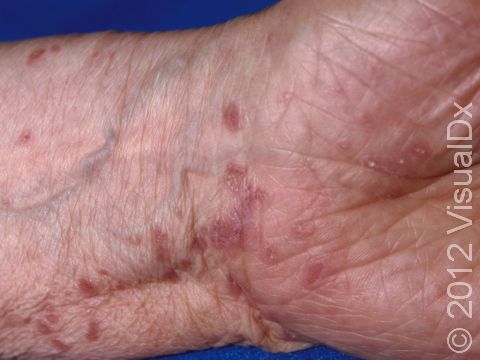
Here is what you should expect: During the visit, your dermatologist will ask you about the duration and progression of hair loss, including location and extent of hair loss. After clinical history and visual inspection of your hair and scalp condition, dermatologists may use other tools such as dermoscopy and/or scalp biopsies to take a closer look. It is important to alert your physician to any other skin lesions you may have. For example, frontal fibrosing alopecia can be associated with another cutaneous disorder called lichen planus pigmentosus that most commonly presents as slate gray to brown-black macules that emerge in sun-exposed areas, often on neck and face1.
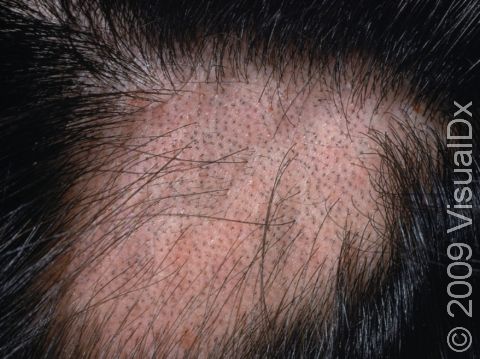
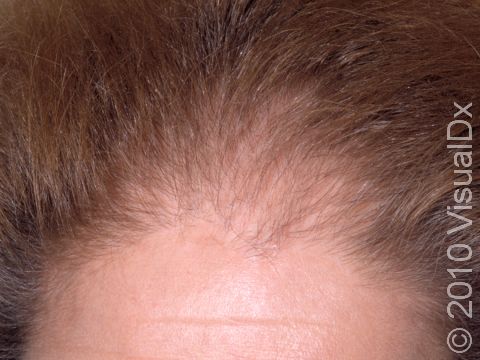
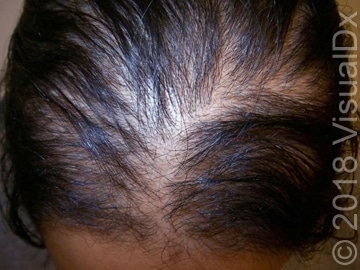
There are two major categories of hair loss to be aware of: scarring (cicatricial) or non-scarring (non-cicatricial). Non-scarring hair loss is more common than scarring hair loss. What causes hair loss scarring? A lack of follicular ostia suggests a scarring alopecia, where hair follicles are destroyed and will most likely not grow back2. Female pattern hair loss, or androgenetic alopecia, is a common form of non-scarring hair loss in adult women. Patients with this type of hair loss will notice a thinning of hair due to a decrease in the normal terminal hair diameter in the frontal and vertex regions of the scalp. The hairs stay in the growth phase for a shorter period of time, becoming thinner and shorter intermediate or vellus hairs in the frontal and vertex regions of the scalp. Other types of hair loss include two other common forms of scarring hair loss: central centrifugal cicatricial alopecia and frontal fibrosing alopecia. Traction alopecia is a common form of hair loss seen on the frontal hairline and temples primarily in African American women.
After making a diagnosis, your dermatologist will work with you to find the best treatment. For example, patients with mild symptoms due to female pattern hair loss (androgenetic alopecia) are usually first treated with minoxidil 5%. An important point you must remember is that your hairs are growing at various phases in an asynchronous pattern. Therefore, be diligent to apply minoxidil consistently over at least four to six months, sometimes at least one year, before expecting any improvement. Show your dermatologist how you apply the minoxidil to ensure a correct application technique. Amy J. McMichael, MD, chair and professor of Department of Dermatology at Wake Forest Baptist Medical Center, teaches her patients a “5 lines, 90 seconds” rule, where patients apply the foam in five streaks on the scalp, the process lasting no longer than 90 seconds. Recent reports have also shown that low-level laser light therapies, or photomodulations, have improved hair loss3,4. In female patients with moderate hair loss due to androgenic alopecia treatments include finasteride, spironolactone, flutamide, and more recently, oral minoxidil can be prescribed. Hypertrichosis, an excessive hair growth above normal, can be a side effect in some patients using oral or topical minoxidil. Lastly, patients with severe hair loss may try hair restoration surgery, platelet rich plasma or wigs. Trials for platelet-rich plasma5 and prostaglandin-2 inhibitors6 are underway for treatment of androgenetic alopecia and alopecia areata (patchy balding).
While consistent use of treatment is key, it is just as imperative to avoid physical damage from chemical relaxants and heat, which can cause hair fragility and hair loss. No matter the severity of your hair loss, you can do your part by being gentle with your hair!
Sources:
1. Rao R, Sarda A, Khanna R, Balachandran C. Coexistence of frontal fibrosing alopecia with lichen planus pigmentosus. Int J Dermatol. 2014;53(5):622-624. doi:10.1111/j.1365-4632.2012.05630.x.
2. Bergfeld WF. Alopecia: histologic changes. Adv Dermatol. 1989;4:301-320.
3. Perper M, Aldahan AS, Fayne RA, Emerson CP, Nouri K. Efficacy of fractional lasers in treating alopecia: a literature review. Lasers Med Sci. 2017;32(8):1919-1925. doi:10.1007/s10103-017-2306-7.
4. McMichael AJ. Excimer laser: a module of the alopecia areata common protocol. J Investig dermatology Symp Proc. 2013;16(1):S77-9. doi:10.1038/jidsymp.2013.31.
5. Ferrando J, García-García SC, González-de-Cossío AC, Bou L, Navarra E. A Proposal of an Effective Platelet-rich Plasma Protocol for the Treatment of Androgenetic Alopecia. Int J Trichology. 9(4):165-170. doi:10.4103/ijt.ijt_27_17.
6. Keaney T. Emerging Therapies for Androgenetic Alopecia. J Drugs Dermatol.2015;14(9):1036-1040. http://www.ncbi.nlm.nih.gov/pubmed/26355625. Accessed December 4, 2017.
Last modified on July 6th, 2023 at 11:01 pm