Uncovering the Benefits & Risks of Topical Steroid Use
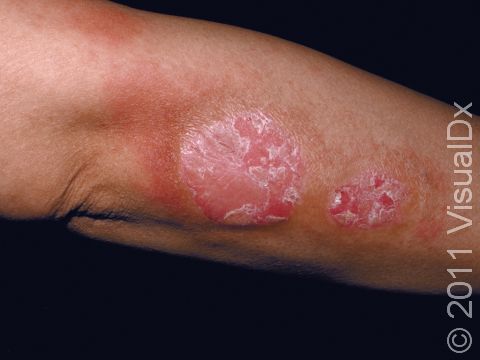
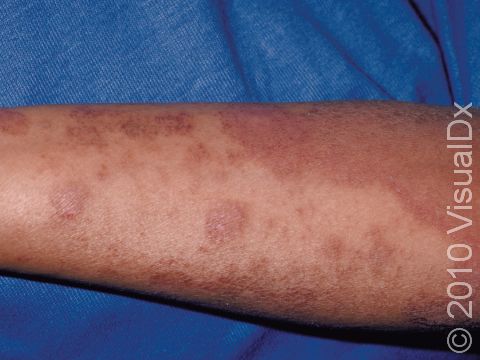
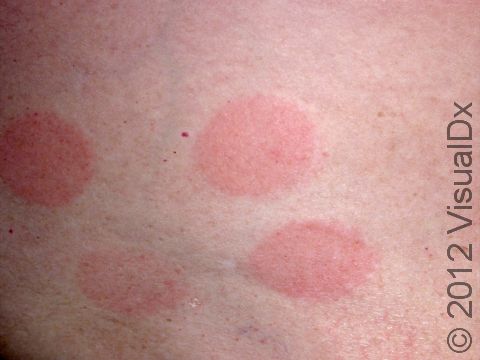
Dermatologists have many strategies and tools available to treat skin conditions. One treatment that is very common in dermatology clinics is prescribing topical steroids. Steroids are used to treat common skin conditions such as eczema, psoriasis, and contact dermatitis. However, many patients wonder why they are being prescribed a topical steroid and how these medications can improve their skin conditions. In order to understand how topical steroids work, let’s break down both words individually.
Topical medications are medicines that can be applied directly to the skin. They come in many forms such as creams, lotions, gels, oils, sprays, and more. Topical treatments start working after they are absorbed through the skin, acting locally and affecting mostly the areas where they are applied. Topical medicines are ideal when we want the medicine to act in limited areas of the skin while minimizing its effects on other organs throughout the body. We can contrast topical medications with oral or injectable medications, which aren’t as selective and often exert their effects on all kinds of tissues. In dermatology, topical medications are ideal as they can act on specific areas of skin with less effect on the rest of the body.
Now that we understand what topical means, let’s break down the term steroid. Many patients may get concerned when they hear the word steroid as the word can have many meanings as well as potentially negative associations. Commonly, patients will hear stories about anabolic steroid use in athletes and may mistakenly think that anabolic steroids are the same thing as the corticosteroids used in dermatology. The confusion comes from the fact that a steroid isn’t just one thing, but rather a broad category of molecules with many families that have different functions. In dermatology, we often use corticosteroids, which are particularly useful in calming down the immune system. These steroids are made in a laboratory, but they accomplish the same purpose as the steroids that our own body makes in times of stress (cortisol).
Our body is primed to produce corticosteroids in times of stress or peril. In our ancestors, cortisol would be released in response to extreme danger, such as if they encountered a wild animal and needed to run for their lives. In modern times, we have far fewer life-threatening situations, but our bodies still produce extra cortisol in other types of stressful situations. These triggers can range from getting cut off in traffic to having to speak in public. The release of cortisol as part of the fight-or-flight response was very important for the survival of our ancestors, but how does this relate to dermatology?
Corticosteroids have some interesting effects on the body, most of which are helpful in situations where you would need to escape from danger. They can increase your blood pressure and blood sugar, which are very important for someone running for their life. In dangerous situations, your body will need all the energy it can get and can’t be wasting resources on anything not necessary at that moment. Cortisol helps accomplish that by toning down certain processes in your body that take a lot of energy to maintain. Your immune system consists of many cells that use a lot of energy, and steroids are very powerful in their ability to put these inflammatory processes on hold.
Many dermatological diseases are related to a dysfunctional or overactive immune system. If we have a way to “tone down” a person’s immune system, we can treat a lot of common skin conditions. If a skin disease is located on certain areas of the body, we can apply topical corticosteroids to those areas to calm down the immune system and improve the skin condition. That’s why topical corticosteroids have become a popular tool for dermatologists to use in treating patients. After reading this article, I hope that you have a better understanding of what topical steroids are and why your dermatologist may prescribe them!
Michael Ryan is a PGY-3 Dermatology Resident at The University of Texas Health Science Center at Houston, McGovern Medical School. He enjoys working as a medical volunteer and giving presentations at local schools about sun protection.
Last modified on August 31st, 2023 at 4:03 pm