Hidradenitis Suppurativa
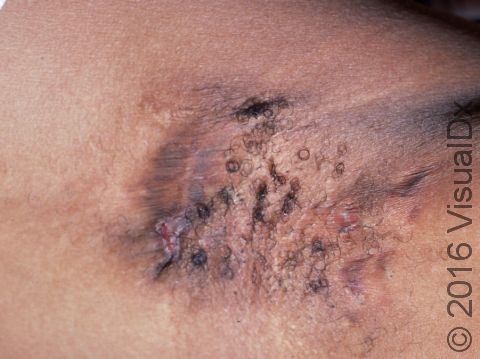
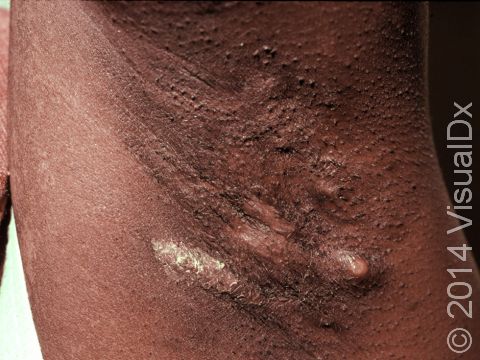
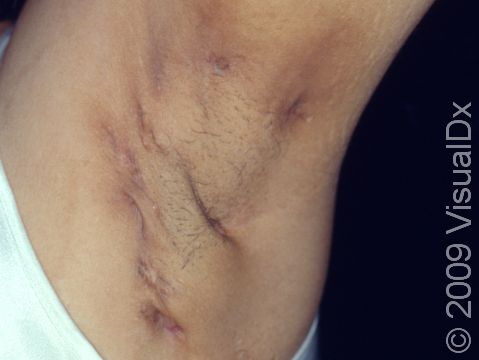
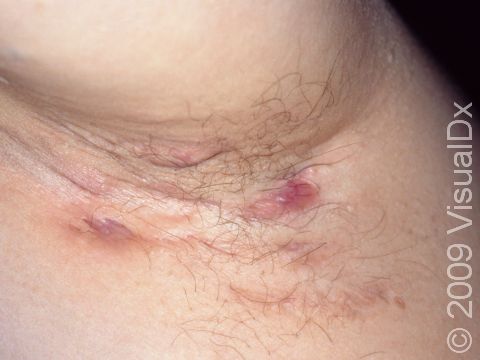
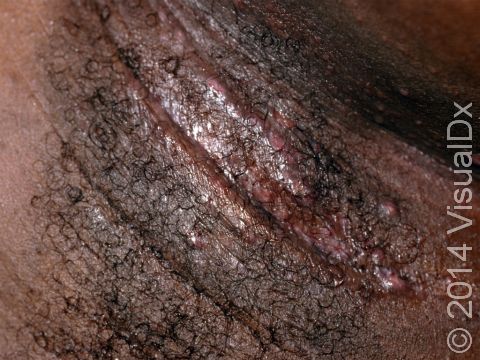
Hidradenitis suppurativa (HS) is a chronic condition of clogged sweat glands that leads to inflammation of the skin in areas such as the groin, underarms, underneath the breasts, and in between the buttocks. It most commonly appears as multiple large nodules (solid, raised bumps), abscesses (red, swollen, warm, tender bumps or lumps with pus inside), and tunnels (holes in the skin that may contain fluid such as pus) in these areas. The nodules and abscesses gradually get larger and drain pus. After multiple bouts of this cycle of plugging, enlargement, and drainage, there may be tunnel formation under the skin and scarring. Pain is the most common symptom, but individuals with HS also report itchy lesions, a foul odor coming from lesions when they drain pus, feeling tired, and joint pain.
While there is no cure for HS, you can work with your medical professional to treat existing lesions and help prevent new ones.
Who's At Risk?
HS usually starts soon after puberty and continues into adult life. It is more common in women and in Black individuals. Hair removal from shaving or using depilatories, deodorants, and irritation from anything rubbing against the affected area can worsen the condition. HS is often associated with smoking, obesity, diabetes, and hormonal changes. Additionally, it often runs in families.
Signs & Symptoms
The lesions of HS are firm, tender bumps. In lighter skin colors, the lesions are often pink or red. In darker skin colors, the lesions may appear brown, purple, or gray. There may also be tunneling under the skin and scar formation. There may be blackheads within scars, and the lesions may drain pus. The groin and underarms are often affected. There may also be lesions between the buttocks or under the breasts. HS lesions are occasionally seen on the trunk of the body or on the scalp or legs.
Some people may experience only one or a few lesions, while others may have severe disease, affecting many areas.
People with HS may experience depression and anxiety, especially if the disease is severe or chronic.
Self-Care Guidelines
Wash draining areas of HS with antibacterial soap or a cleanser containing benzoyl peroxide, chlorhexidine, or zinc pyrithione. Then apply an antibiotic ointment (eg, Neosporin) and cover with a clean bandage. If there is a large amount of drainage, use gauze pads under bandages and change them often. Warm compresses and ibuprofen (eg, Advil, Motrin) can help reduce the pain and swelling.
To help prevent further irritation, avoid wearing tight-fitting clothing and try to avoid friction to affected areas of skin.
Weight loss may decrease lesions by eliminating skin folds and, thus, friction on the skin. Stop smoking, if applicable.
Treatments
Your medical professional will recommend the treatment or treatments that are best for your HS.
For small HS flare-ups in one body location, your medical professional may inject steroids into the area. Oral antibiotics are often used as first treatments for flare-ups or long-term control. Oral steroids may be used for widespread flare-ups or to help as a “bridge” until other long-term treatments are effective.
If hormonal fluctuations are thought to be contributing to the condition, you may be prescribed hormonal therapy, such as oral contraceptives, or spironolactone.
Biologic medicines such as adalimumab can be used when first-line treatments don’t work or as first-choice therapy for severe cases.
Surgery is often used for areas with chronic, persistent inflammation, especially tunnels.
Visit Urgency
Some mild cases of HS can be treated with self-care measures. Healing of individual lesions takes about 1-2 weeks. However, seek medical care if the pain isn’t controlled with ibuprofen and warm compresses or if the condition is making you feel sad, anxious, or avoid going out in public. Medical treatment may be necessary if the condition appears in multiple body locations or continues to come back.
If there is excessive pain, excessive drainage, red streaking, you have a fever, or there are any other factors that may indicate there is an infection, see your medical professional.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on April 3rd, 2026 at 1:05 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder