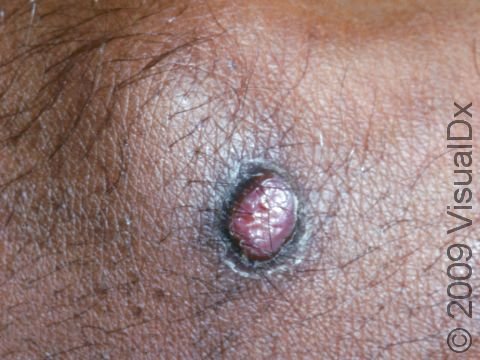
Lobular Capillary Hemangioma (Pyogenic Granuloma)
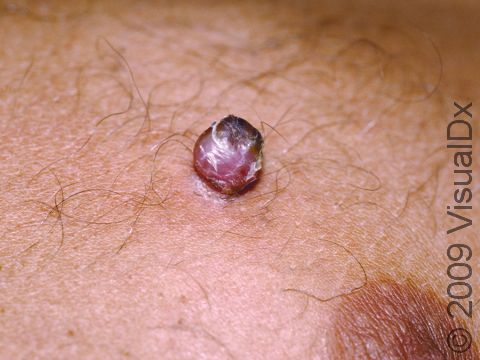
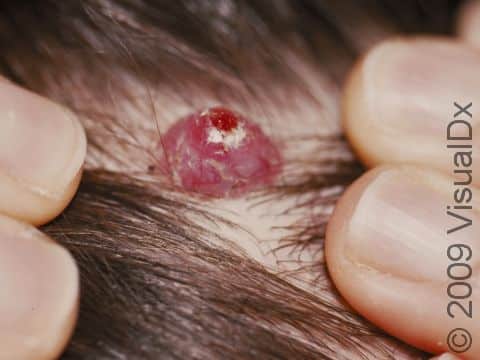
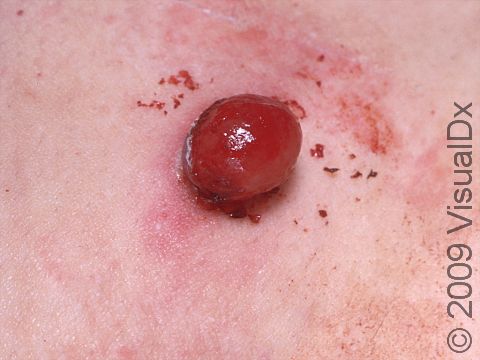
Lobular capillary hemangiomas, also known as pyogenic granulomas, are common, harmless growths that can appear on the skin, the lips, and inside the mouth. They are composed of blood vessels and may occur at the site of a minor injury. They may also be caused by certain medications (eg, isotretinoin) and medical therapies (eg, laser treatment). They often grow rapidly, within weeks. They can bleed easily, especially if injured.
When a lobular capillary hemangioma occurs during pregnancy, it is sometimes called a “pregnancy tumor” (granuloma gravidarum). Lobular capillary hemangiomas develop in up to 5% of pregnant women.
Who's At Risk?
Lobular capillary hemangiomas occur in people of all races / ethnicities. Women are more frequently affected by lobular capillary hemangiomas than men, although male and female children are equally affected.
Lobular capillary hemangiomas are most often seen in:
- Children and young adults.
- Pregnant individuals.
- People taking oral contraceptives.
- People taking certain oral retinoid medications, including isotretinoin or acitretin.
- People taking protease inhibitors such as indinavir.
- People undergoing chemotherapy.
Signs & Symptoms
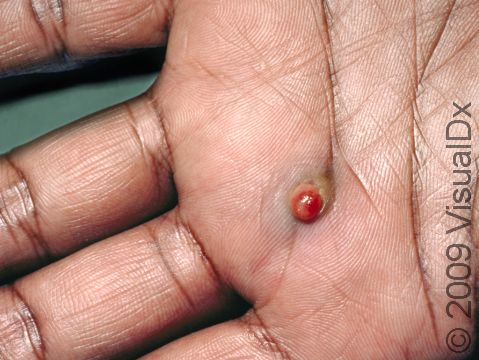
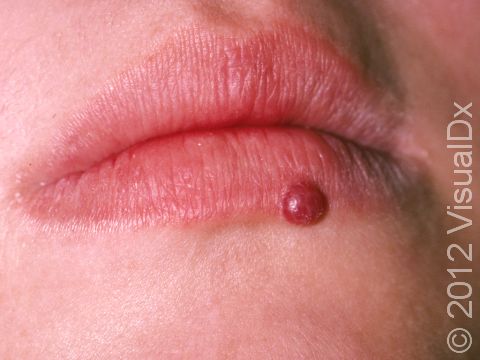
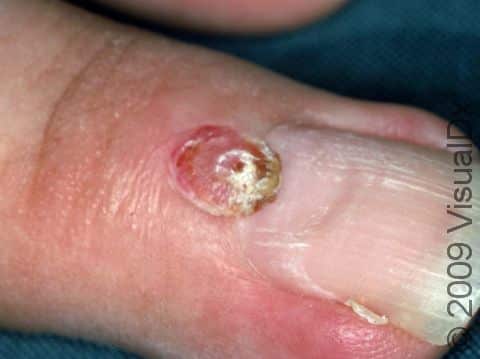
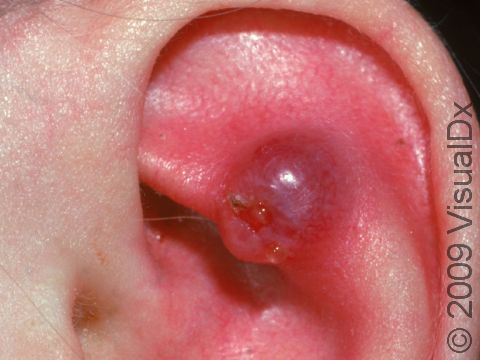
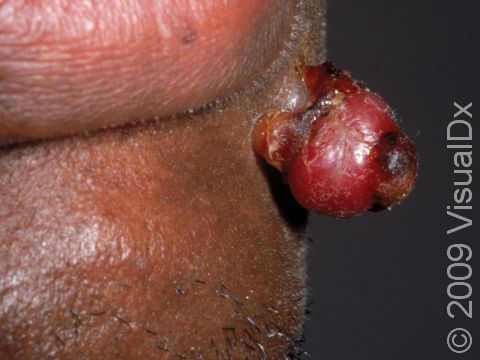
Typically, a lobular capillary hemangioma appears as a bright red papule (small, solid bump) or nodule (solid, raised bump) that enlarges rapidly over a few weeks. Lobular capillary hemangiomas are usually 5-10 mm in diameter. They may bleed easily and can be tender. They may scab after bleeding. Rarely, more than one lobular capillary hemangioma may develop at the same time.
The most common locations for lobular capillary hemangiomas include the:
- Lips, gums, and inner mouth (particularly in pregnant individuals).
- Hands and fingers.
- Head and neck.
- Feet and toes.
- Upper trunk.
Self-Care Guidelines
See your medical professional if you notice any rapidly enlarging skin growth to establish the correct diagnosis. Because lobular capillary hemangiomas are prone to easy bleeding, it can help to cover the lesion with a bandage until you see your medical professional.
Treatments
If the diagnosis of lobular capillary hemangioma is suspected, your medical professional may perform a skin biopsy to confirm the diagnosis.
Sometimes, lobular capillary hemangiomas may go away on their own. Those that develop during pregnancy often resolve after delivery. Similarly, lobular capillary hemangiomas associated with medications usually improve when the medicine is stopped or the dosage is lowered. Depending on the size of the lobular capillary hemangioma and its location and symptoms, your medical professional may decide that no treatment is necessary.
But these lesions are frequently removed because they can bleed, become tender, and can be cosmetically bothersome.
Treatments include:
- Shave removal or curettage (scraping) followed by electrocautery (burning with an electric needle).
- Applying a chemical substance (silver nitrate) that will cause flattening of the lesion.
- Freezing with liquid nitrogen (cryotherapy).
- Laser treatment.
Lobular capillary hemangiomas can come back after treatment, especially those lesions located on the trunk of teenagers and young adults. Recurrent lobular capillary hemangiomas are best treated by surgical excision.
Visit Urgency
Make an appointment with a dermatologist or another medical professional if any rapidly enlarging or bleeding growth develops on your skin or in the areas lining your nose or mouth (mucous membranes).
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 17th, 2024 at 2:55 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder