Yeast Infection (Candidiasis)
Candidiasis, commonly known as a yeast infection, is an overgrowth of the common Candida albicans fungus, which is naturally found in the environment and on the body. Sometimes this yeast lives in the mouth, digestive tract, and the vagina without causing any issues. However, under certain conditions (such as having a weak immune system, using antibiotics, taking cancer drugs or corticosteroids, or being obese or diabetic), the yeast will multiply and cause an infection.
There are different forms of yeast infection, depending upon the area affected. Most commonly, the mouth, vulva and vagina, and damper skin areas, such as the skin folds, are affected, as the yeast likes to grow in moist environments.
Most yeast infections are easily treated; however, serious life-threatening yeast infection can develop throughout the body (systemically) in people with very weak immune systems.
Who's At Risk?
Various species of Candida yeast grow in over half of healthy adults.
- Men and women can both get yeast infections.
- People with weakened immune systems; those taking antibiotics, cancer drugs, or corticosteroids; those with diabetes; and those who are obese are most likely to develop a yeast infection.
- Older people are more likely to get thrush (oral yeast infection).
- Yeast infection is a common cause of inflammation of the vagina (vaginitis).
Signs & Symptoms
The appearance and symptoms of yeast infection depend upon the area affected. Usually, the affected area is itchy.
The most common types of infection are:
- Thrush – The mouth lining, tongue, and/or corners of the mouth are red, cracked, or have white patches. There may be soreness or there may be no symptoms.
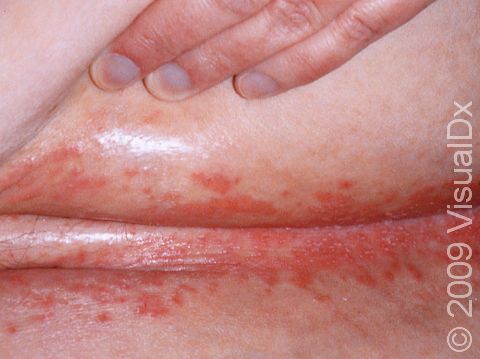
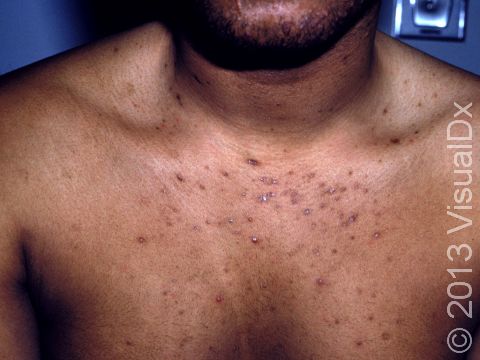
- Skin (cutaneous) – Small-to-large patches of red, moist, raw skin usually develop in body creases, such as under the breasts, belly, or groin area. The skin may itch or be painful. Tiny pustules (pus-filled bumps) may appear around the edges of the red areas. In darker skin colors, the area may be dark red, purple, dark brown, or grayish.
- Vaginitis – Vaginal itch, pain, and burning are frequent and may be accompanied by a cottage-cheese-like discharge. There is usually pain with sexual intercourse.
- Esophagitis – Swallowing may be painful, and there may be pain behind the breastbone.
Self-Care Guidelines
- Most skin yeast infections can be prevented by keeping body folds clean and dry.
- Avoid wearing tight-fitting clothing.
- Treat skin yeast infection with an over-the-counter antifungal cream (such as clotrimazole or miconazole) twice daily for 10-14 days.
- Those with vaginitis can use an over-the-counter vaginal suppository or cream antifungal (miconazole or clotrimazole). Avoid sexual intercourse until the yeast infection heals. If you are pregnant and have a vaginal yeast infection, consult your medical professional for treatment guidance.
- Individuals with diabetes should keep their blood sugar under good control.
- For those who are overweight, losing weight can help prevent yeast infection from recurring.
Treatments
Your medical professional may prescribe a topical or oral antifungal medication in addition to the self-care measures noted above.
Visit Urgency
See your medical professional if your symptoms do not go away with self-care.
Note that vaginitis can be caused by other infections or inflammatory conditions. If you are sexually active and are having symptoms such as those above, you may have a sexually transmitted infection. See your medical professional to confirm the diagnosis.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 17th, 2024 at 8:49 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder