Keratosis Pilaris
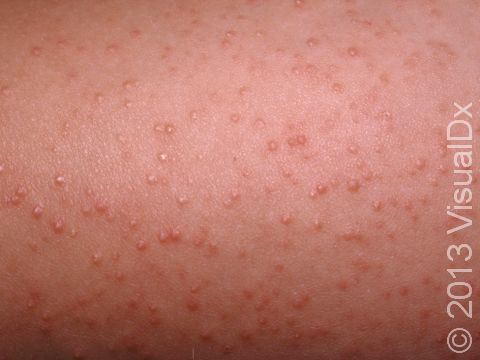
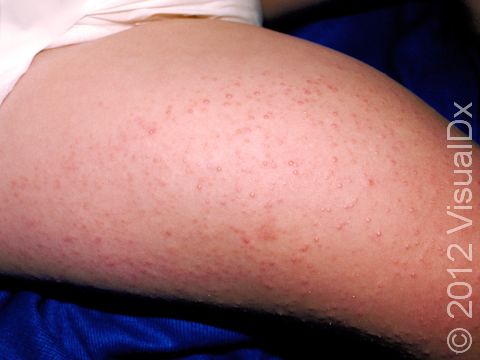
Keratosis pilaris is a very common, harmless skin condition appearing as rough, whitish papules (small, solid bumps) on the upper arms and thighs, especially of children and young adults.
Individual lesions of keratosis pilaris begin when a hair follicle becomes plugged with keratin, a protein found in skin, hair, and nails.
Who's At Risk?
Keratosis pilaris can affect people of any age, race, and sex. It is more common in females.
Keratosis pilaris usually starts in early childhood (by age 10) and can worsen during puberty. However, it frequently improves or even goes away by early adulthood.
Keratosis pilaris can affect 50%-80% of teenagers and up to 40% of adults. Many people have a family history of keratosis pilaris. A large proportion of individuals with ichthyosis vulgaris (an inherited skin condition characterized by very dry, very scaly skin) also report having keratosis pilaris.
Signs & Symptoms
The most common locations for keratosis pilaris include the following:
- Back of the upper arms
- Front and sides of the thighs
- Buttocks
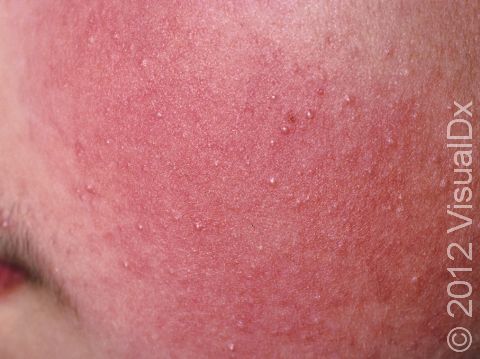
- Cheeks
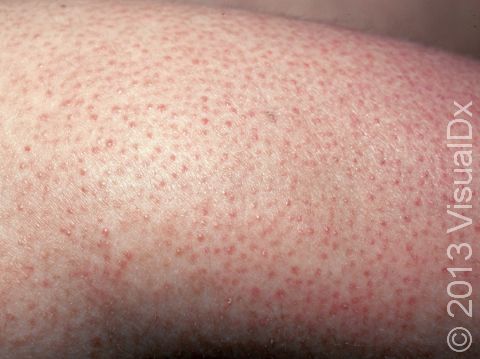
Keratosis pilaris lesions are tiny (1 mm) white-to-gray bumps centered in the hair follicle. Sometimes a thin, red ring may surround the white bump, indicating inflammation. In darker skin colors, the red area around the bumps may be harder to see or may be darker brown. The bumps all look very similar to one another, and they are evenly spaced on the skin’s surface.
Rarely, people with keratosis pilaris may experience mild itching.
Keratosis pilaris tends to improve in warmer, more humid weather, and it may worsen in colder, drier weather.
Self-Care Guidelines
There is no cure for keratosis pilaris, but its appearance can be improved. It is often helpful to keep the skin moist (hydrated) and to use mild, fragrance-free cleansers, with daily applications of moisturizer.
Creams and ointments are better moisturizers than lotions, and they work best when applied just after bathing, while the skin is still moist. The following over-the-counter products may be helpful:
- Preparations containing alpha-hydroxy acids such as glycolic acid or lactic acid (eg, CeraVe SA Cream for Rough & Bumpy Skin)
- Creams containing urea (eg, Cetaphil Rough & Bumpy Daily Smoothing Moisturizer)
- Hydrocortisone (eg, Cortaid) 1% cream (if the areas are itchy)
Do not try to scrub the bumps away with a pumice stone or similar harsh material; these approaches may irritate the skin and worsen the condition. Similarly, try to discourage your child from scratching or picking at the bumps, as these actions can lead to bacterial infections or scarring.
Treatments
Keratosis pilaris usually improves with time. However, it is generally considered to be a long-lasting (chronic) skin condition. Treatments are aimed at controlling the rough bumps, not curing them. Keratosis pilaris bumps will come back if therapy is stopped.
To treat the bumps of keratosis pilaris, your child’s medical professional may recommend a topical cream or lotion containing:
- Prescription-strength alpha- or beta-hydroxy acids (glycolic acid, lactic acid, salicylic acid).
- Prescription-strength urea (Carmol, Aluvea, Keralac).
- A retinoid such as tretinoin (Retin-A) or tazarotene (Avage, Tazorac).
- Prescription-strength hydrocortisone cream if inflammation is present.
Visit Urgency
Keratosis pilaris is not a serious medical condition and it has no health implications. However, if self-care measures are not improving the appearance of the skin and it continues to bother your child, see a dermatologist or another medical professional, who may prescribe stronger treatments. If pus-filled bumps appear, that indicates a secondary bacterial infection, and it is also important to seek care if this occurs.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 13th, 2024 at 10:49 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder