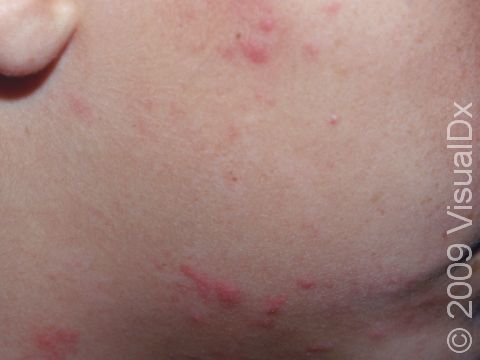
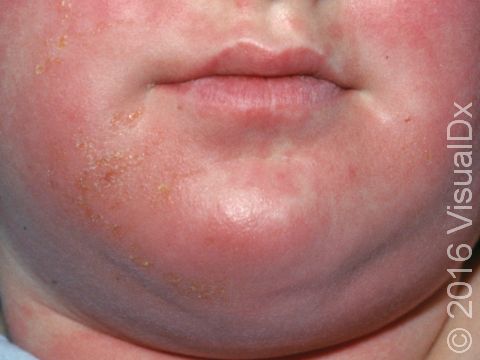
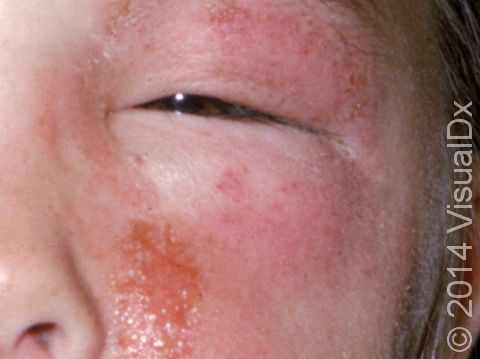
Poison Ivy, Oak, and Sumac
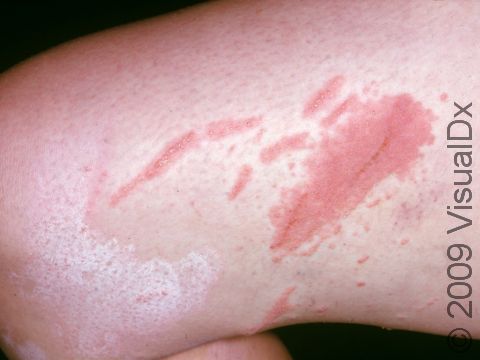
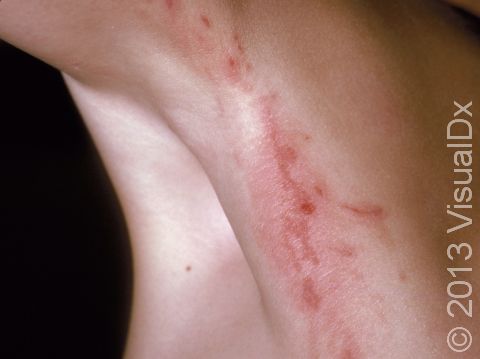
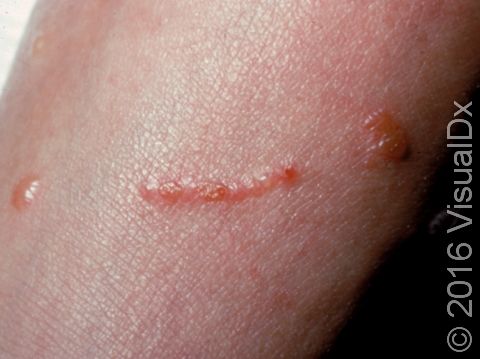
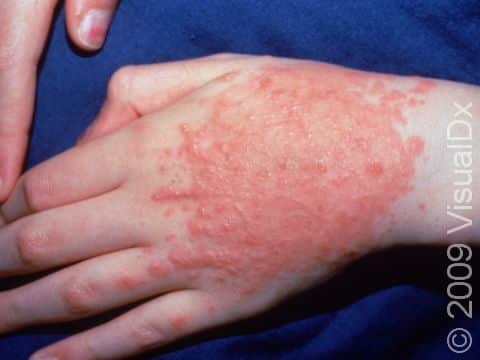
Poison ivy, poison oak, and poison sumac rashes (dermatitides) are all an allergic reaction to the oily resin found on the leaves, stems, and roots of poison ivy, poison oak, and poison sumac plants, called urushiol. The allergy starts after repeated exposure to the plant’s oil and may occur at any age. People usually develop an itchy rash of papules (small, solid bumps), plaques (a raised or bumpy area larger than a thumbnail), vesicles (small blisters), and sometimes bullae (blisters larger than a thumbnail) in the affected areas.
- The itch can be intense, and scratching may break the skin, resulting in bacterial infection.
- You cannot spread the rash from touching the lesions, even if the blisters pop; the rash is spread by contact with the plant resin itself.
- The rash first appears on the areas of skin exposed to the most oil, and then areas exposed to less oil begin to develop a rash later.
- Skin lesions usually begin to appear within 48 hours after exposure if your child has had previous contact with urushiol. If it is their first exposure, the reaction could take up to a few weeks.
Who's At Risk?
Poison ivy, poison oak, and poison sumac may affect people of any age, sex, and race / ethnicity.
Signs & Symptoms
- Poison ivy, poison oak, and poison sumac can occur anywhere on the body where exposure to the plant’s oil has occurred. The arms, legs, face, and neck are commonly affected. Red and brown-red papules, plaques, and blisters appearing in straight lines may be seen, and a crust may form on top. In darker skin colors, the redness may be harder to see, or it may appear more purple or gray.
- In a type of reaction called the “black spot” variant, the oil from the plant leaves one or more black dots on the skin.
- If the face or genitals have been exposed, extreme swelling may develop in the affected area.
- The rash may last for weeks.
Self-Care Guidelines
- After known poison ivy, poison oak, or poison sumac exposure, use warm water to wash all potentially exposed areas within 20 minutes to remove the plant’s oil. Be sure to wash under the nails as well. Once the oil has been washed off, there is no risk of spreading the condition to other parts of the body.
- Be sure to wash clothes, gloves, and shoes that have come into contact with the oil as well.
- Wear protective clothing (long-sleeved shirts, pants, and long socks) to avoid future reactions, or apply a protective barrier (eg, IvyX Pre-Contact Poison Skin Solution).
- Cool tap water, soothing oatmeal baths (Aveeno Soothing Bath Treatment), and calamine lotion can help relieve itch.
- Over-the-counter 1% hydrocortisone cream can be used for mild cases.
- Oral antihistamines (chlorpheniramine or diphenhydramine [eg, Benadryl]) can help relieve the itch, but these may cause drowsiness.
- DO NOT USE topical anesthetics containing benzocaine (eg, Anbesol) or diphenhydramine (eg, Benadryl), as people easily become allergic to these products.
Treatments
Your child’s medical professional may prescribe:
- A medium-to-high-potency topical steroid to treat the trunk and arms and legs or low-potency topical steroid to treat the face and skinfold areas if the affected areas are more limited.
- Prescription oral antihistamines for itching.
- A 14-to-20-day course of oral prednisone if they have a severe outbreak affecting large body areas.
- Topical or oral antibiotics if bacterial infection is present.
Visit Urgency
See your child’s medical professional if the rash does not improve with self-care measures or appears to be getting worse.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 26th, 2024 at 2:49 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder