Postinflammatory Hyperpigmentation
Postinflammatory hyperpigmentation is darkening of the skin in an area of prior injury or inflammation from increased pigment (melanin) left from the healing process. Acne is a common cause of hyperpigmentation, as is any type of skin injury (eg, scrapes, cuts, burns, insect bites, and chronic rubbing) and many other skin disorders, such as eczema (atopic dermatitis).
Who's At Risk?
Although postinflammatory hyperpigmentation can occur in any age, sex, or race / ethnicity, it is more common and often more severe in individuals with darker skin colors. Postinflammatory hyperpigmentation also lasts longer in individuals with darker skin.
Signs & Symptoms
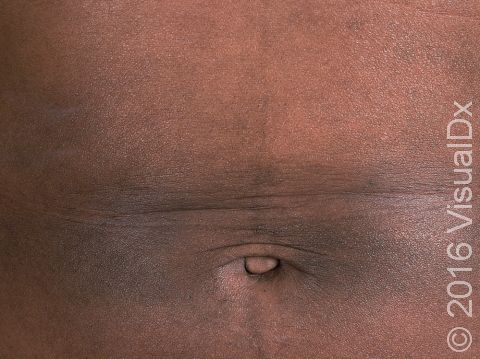
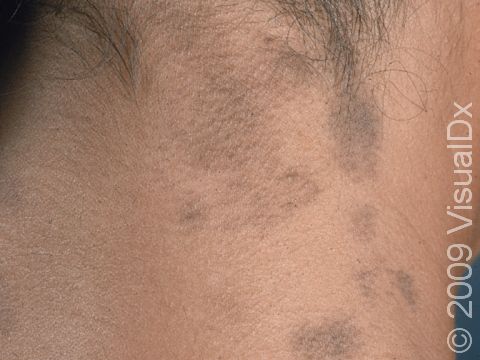
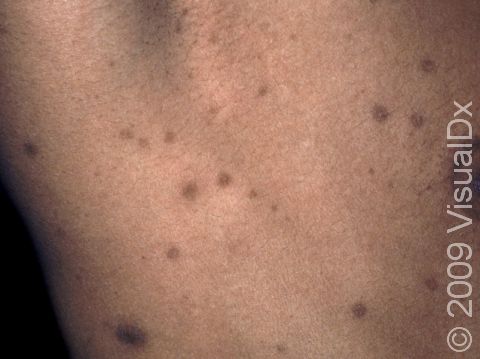
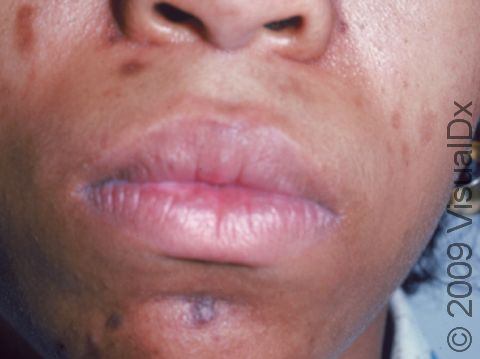
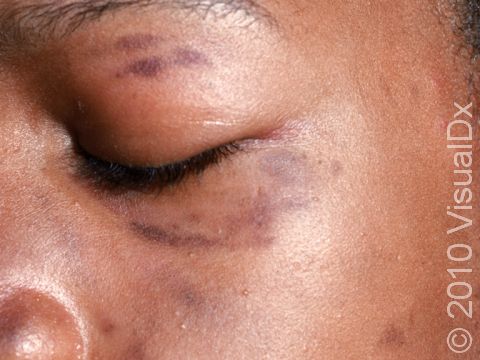
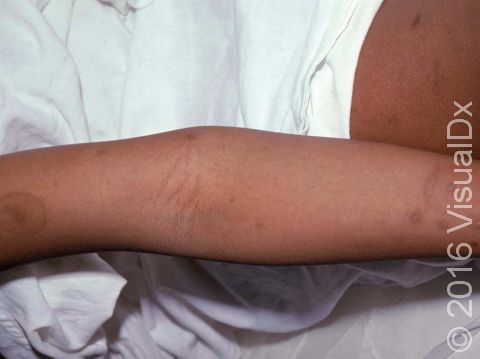
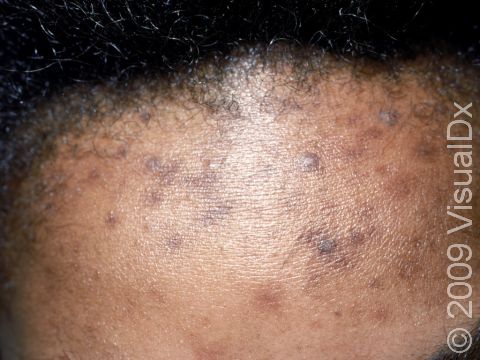
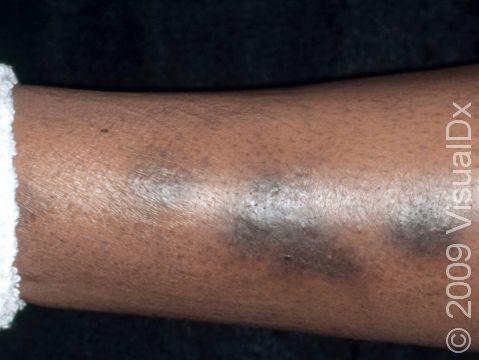
One or more macules (small, flat, smooth areas) or patches (flat, smooth areas larger than a thumbnail) that are darker than the surrounding skin, often appearing as brown or sometimes blue-gray discoloration. Postinflammatory hyperpigmentation varies in size, shape, and location, often in the same shape and size as the initial injury or inflammation. Acne tends to leave light-to-dark-brown macules on the face or trunk. Burns, insect bites, cuts, or scrapes often affect exposed areas on the arms and legs.
In lighter skin, the skin color changes may be subtle or may look more purple than brown.
Self-Care Guidelines
Most postinflammatory hyperpigmentation fades with time, although it may take many months, and some areas never fade (particularly on the legs).
- Avoid picking, scratching, and rubbing the areas as this can prolong the hyperpigmentation or make it worse.
- Sunlight may cause further darkening, so protect yourself from sun exposure with sun-protective clothing, a wide-brimmed hat, and broad-spectrum sunscreen (meaning it blocks UVB and UVA light) with a sun protection factor (SPF) of 30 or higher. For darker skin colors, it is best to use a tinted sunscreen.
- You may be able to use makeup to cover the affected areas. Waterproof makeup is available for use on the face as well as the arms and legs.
- While bleaching creams are available over the counter, the US Food and Drug Administration (FDA) advises against most products containing hydroquinone, as they may worsen pigmentation or cause permanent pigment loss.
Treatments
Some prescription agents may help fade the hyperpigmentation. These include 2%-6% hydroquinone; combination fluocinolone acetonide, hydroquinone, and tretinoin; azelaic acid or other topical lightening agents; and oral tranexamic acid. These products are often used in combination.
Chemical peels, cryotherapy, microdermabrasion, and laser therapy treatments have been used with variable results. In darker skin colors, caution should be used with these sorts of therapies, as they may cause loss of pigmentation, worsening of hyperpigmentation, or scarring.
Visit Urgency
If you have an underlying skin disorder causing hyperpigmentation, such as acne, seek medical care. Also see your medical professional if the hyperpigmentation is bothersome to you.
If you notice any general change in skin color without an obvious explanation, see your medical professional.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 14th, 2024 at 4:01 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder