Scabies (Pediatric)
Scabies is an itchy skin condition caused by a tiny mite called Sarcoptes scabiei that can live and multiply on the skin. Scabies is spread to others through prolonged skin-to-skin contact. Scabies is extremely contagious and spreads rapidly in crowded conditions such as hospitals, child-care facilities, and other situations where people spend extended periods of time in close contact with each other.
The itchy rash of scabies develops when a mite burrows into the outer layer of skin and lays eggs. The human immune system is highly sensitive to the presence of the mite and produces an allergic response that causes intense itching. Although a typical infestation includes only 10-20 mites, people are so sensitive to the mite that hundreds of itchy skin lesions may arise. Without proper medical treatment, the condition will not usually improve.
Who's At Risk?
Scabies is seen in people of all races / ethnicities, ages, and sexes. Scabies is not caused by lack of personal hygiene, but it is common in people who live in crowded conditions.
Other individuals at risk include:
- Children.
- Caregivers of young children.
- Sexually active young adults.
- People living in and working in assisted living facilities.
Although scabies is extremely contagious, it usually requires prolonged skin-to-skin contact with a person already infested. A quick handshake or hug will not normally spread the infestation. However, scabies is easily spread to other members of the same household. It may be spread by sharing towels, clothing, or bedding.
Signs & Symptoms
Although the entire body may itch, the most common locations for the lesions of scabies in older children and adults include the:
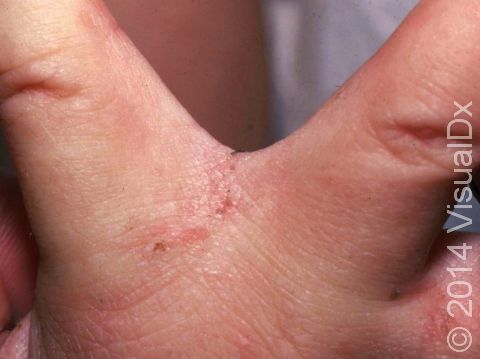
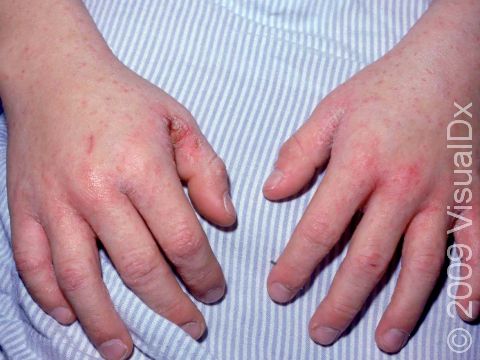
- Areas between the fingers (finger webs).
- Inner wrists, inner elbows, and armpits.
- Breasts of females and genitals of males.
- Belly button.
- Lower abdomen.
- Buttocks.
- Backs of the knees.
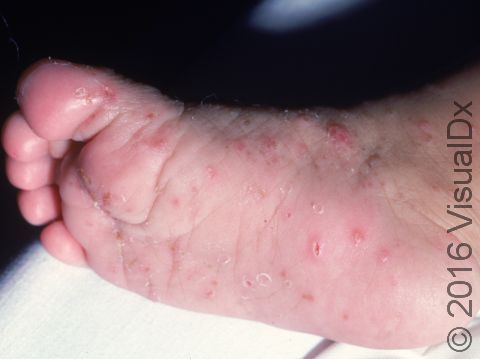
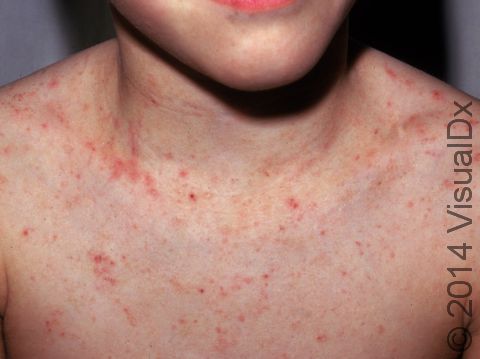
In young children, the lesions of scabies are most commonly seen on the:
- Trunk, arms, and legs.
- Neck.
- Palms of the hands and soles of the feet.
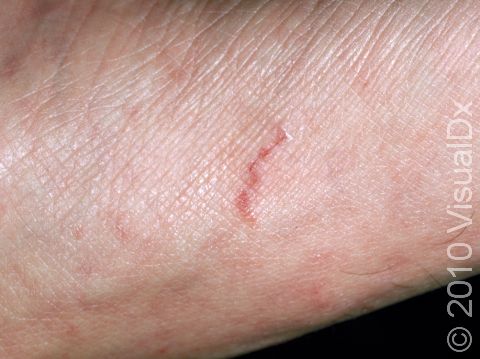
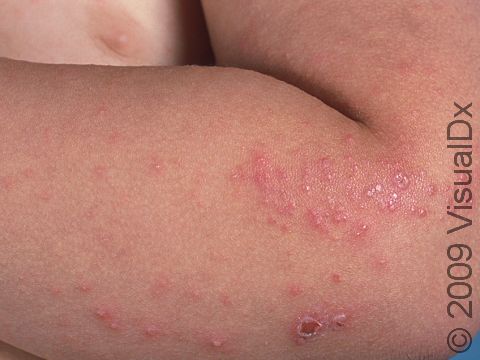
The most obvious signs of scabies are pink-to-red papules (small, solid bumps). In darker skin colors, the redness may be harder to see, or it may appear purple or brown. The papules may be scabbed over from scratching. The telltale sign of scabies is the burrow, which is a fine, thread-like, scaly line (3-10 mm long), sometimes with a tiny black speck (the burrowing mite) at one end. The rash of scabies is intensely itchy, especially at night.
Scratching the itchy lesions can create breaks in the skin, and these breaks can become infected with bacteria.
People who are exposed to scabies may not develop itchy lesions for up to 6 weeks after becoming infested, as the immune system takes some time to recognize the mites and develop an allergic response to them. However, individuals who have had scabies before may develop the rash within several days of re-exposure.
Self-Care Guidelines
Scabies requires prescription medication to stop the infestation. Once your child is being treated, there are steps you can take to remove scabies mites from the household:
- Mites cannot survive off the human body for more than 48-71 hours. Therefore, wash all clothing, bedding, and towels used by the infested person in the previous 72 hours in hot water and dry these items in a hot dryer.
- Vacuum all carpets, rugs, and upholstered furniture, and discard the vacuum bags.
- Put anything that cannot be laundered into plastic bags for at least 72 hours.
Pets do not need to be treated because the mite only lives on humans.
Treatments
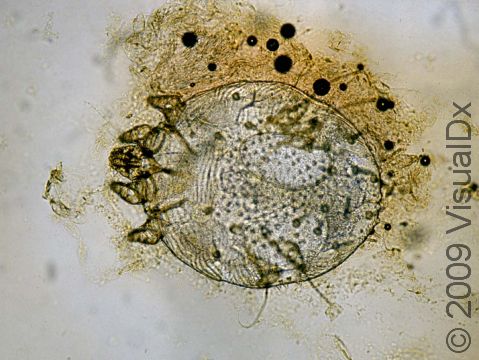
The medical professional may be able to diagnose scabies simply by examining the child’s skin for typical lesions such as burrows. However, they may also want to perform a skin scraping, called a scabies preparation, to look for mites, eggs, or mite feces under a microscope to confirm the diagnosis.
In most cases of scabies, the medical professional may recommend a topical cream or lotion, such as:
- Permethrin cream.
- Lindane lotion or cream.
When using a topical cream, lotion, or ointment, be sure to follow these steps (unless your medical professional gives other instructions):
- Apply to the child’s entire body, from the neck down.
- Smear the product beneath your child’s fingernails and toenails.
- Apply to body folds, including inside the belly button, in the buttocks crease, and between the toes.
For more severe scabies, your child’s medical professional may prescribe oral ivermectin.
The medical professional may prescribe an antihistamine to help relieve itch. If there are scratched areas that appear to be infected with bacteria, they may prescribe oral antibiotics.
Itching may take up to 3 weeks to go away while your child’s immune system continues to react to dead mites. However, new burrows and rashes should stop appearing 48 hours after effective treatment.
Household members and anyone else with prolonged skin-to-skin contact with a person with scabies should seek medical treatment. Since the incubation time for scabies infestations can be from 6-8 weeks, people may be unaware they have scabies. If untreated, these close contacts could pass the mites back to your child. Ideally, everyone should be treated at the same time to prevent re-infestation.
Visit Urgency
See your child’s medical professional for evaluation if the child develops an extremely itchy rash. If other members of the household or your child’s close contacts have similar itchy rashes, they should also be evaluated by a medical professional.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
Centers for Disease Control and Prevention. Scabies Frequently Asked Questions (FAQs). CDC. https://www.cdc.gov/parasites/scabies/gen_info/faqs.html. Updated 2020 Sept 1.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on July 11th, 2025 at 9:28 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder