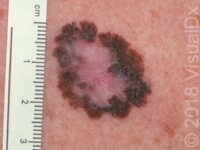
Squamous Cell Carcinoma
Squamous cell carcinoma (SCC) is the second most common form of skin cancer, following basal cell carcinoma. SCC usually occurs on sun-damaged skin, such as the head, neck, arms, and the back of the hands. SCC is most common in individuals with lighter skin colors with a long history of chronic sun exposure.
SCC requires treatment to prevent it from spreading (metastasizing). SCC rarely spreads to lymph nodes or to internal organs. However, if it is neglected, SCC can spread into deeper skin layers or it may spread to other parts of the body.
Another common type of skin cancer is melanoma.
Who's At Risk?
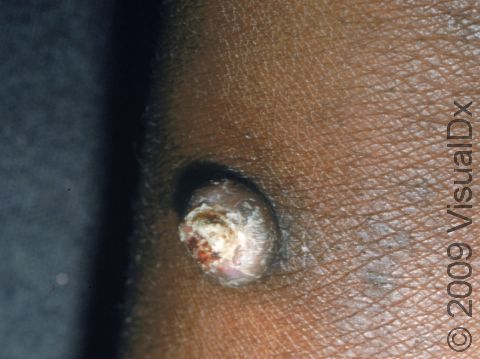
SCC is most commonly seen in older, lighter-skinned individuals following sun exposure. However, anyone can develop SCC, including darker-skinned individuals, especially in scars and chronic skin sores. In fact, SCC is the most common form of skin cancer in Black individuals.
Risk factors for developing SCC include:
- Age over 50 years.
- Light skin, light hair, and/or light eyes.
- Male sex.
- Chronic exposure to sunlight or other ultraviolet (UV) light.
- Exposure to certain chemicals, such as arsenic or tar.
- Exposure to radiation, such as x-ray treatment for internal cancers.
- Long-term suppression of the immune system, such as organ transplant recipients.
- Long-term presence of scars.
- Chronic ulcers.
- Previous skin cancer.
Actinic keratoses, also known as solar keratoses, are small rough or scaly areas of skin due to damage from sun exposure. Some actinic keratoses can turn into SCC.
Signs & Symptoms
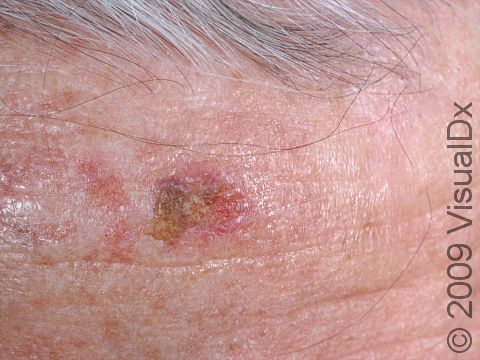
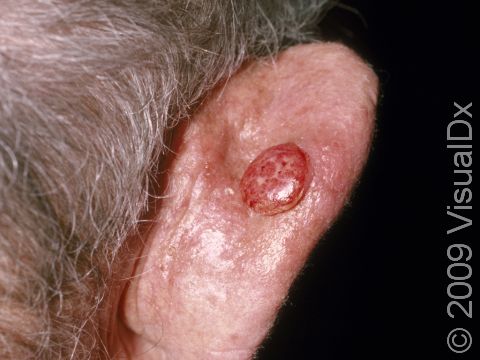
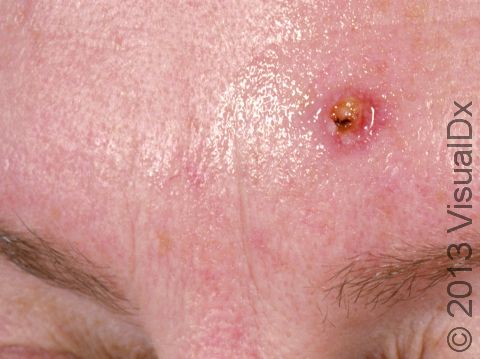
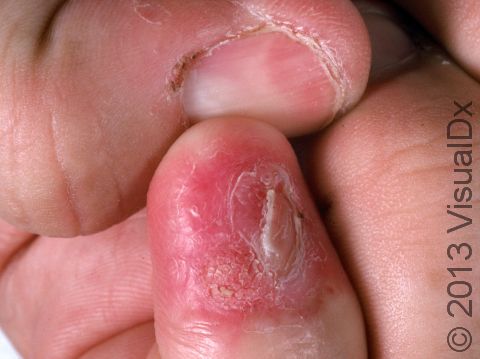
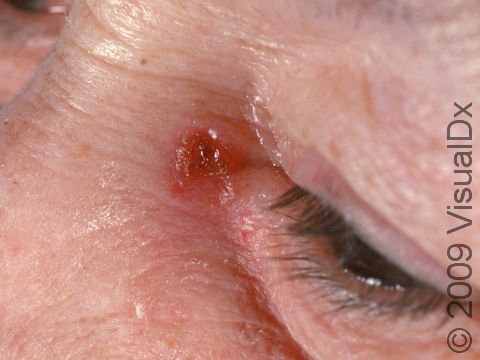
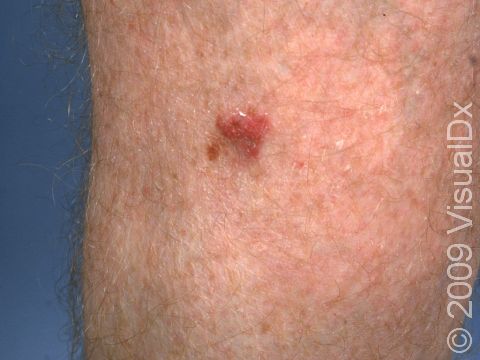
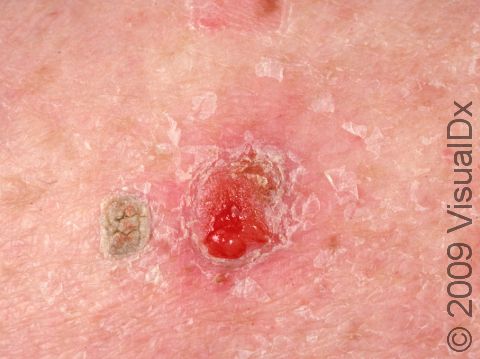
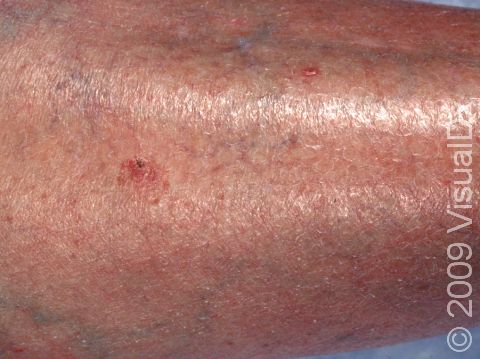
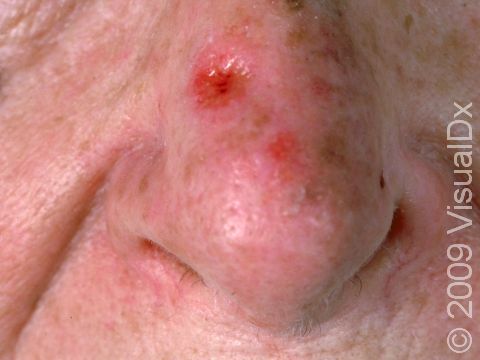
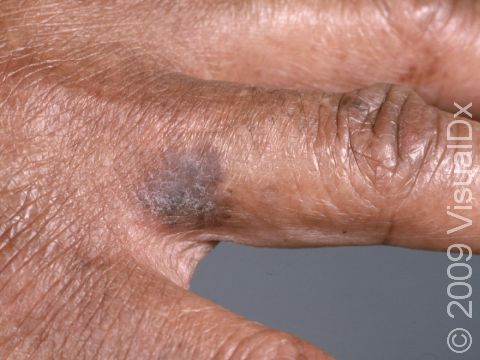
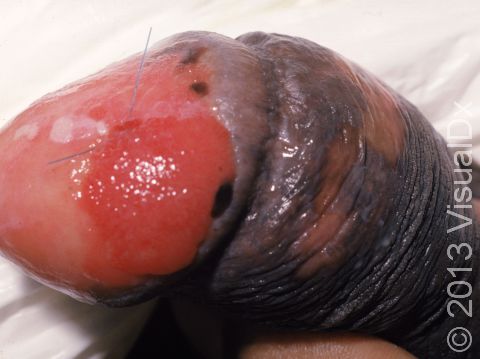
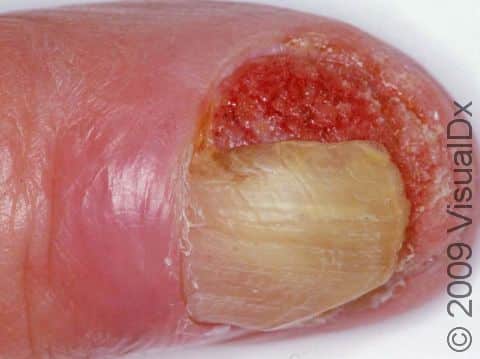
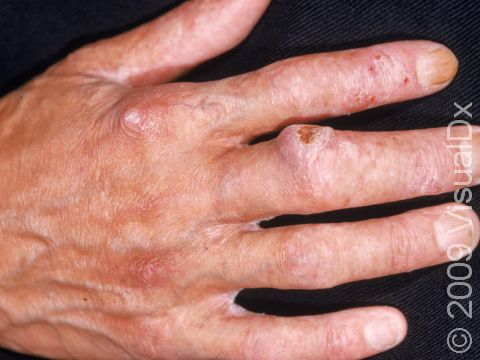
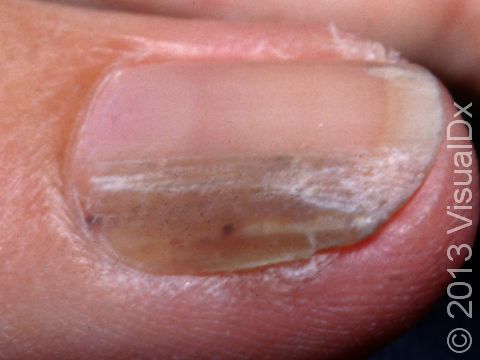
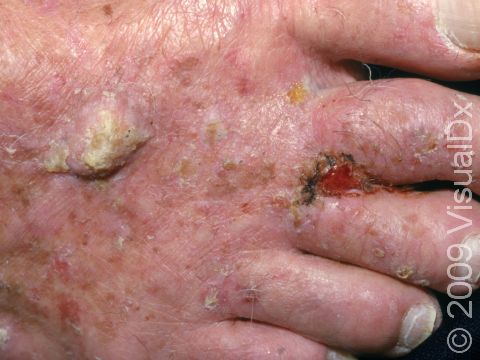
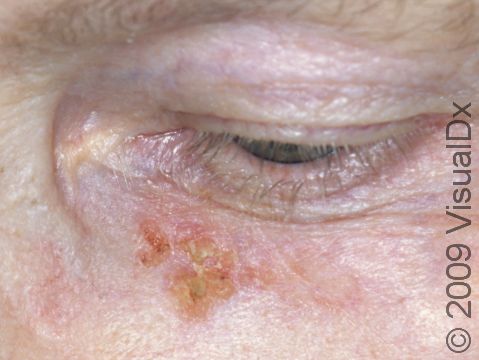
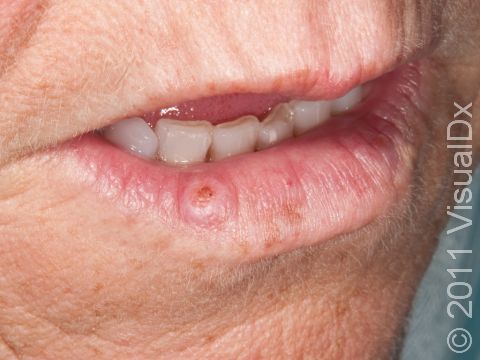
SCC typically first appears as a pink or red, scaly papule (a small, solid bump). It may be painful or painless. Over time, the lesion becomes larger and deeper. Eventually, the center of the SCC forms a sore and may bleed or become scabbed over. In darker skin colors, the redness may be harder to see or the lesion may appear more purple than red.
The most common locations for SCC in lighter skin colors include the:
- Head and neck.
- Arms and hands.
- Shoulders.
- Back.
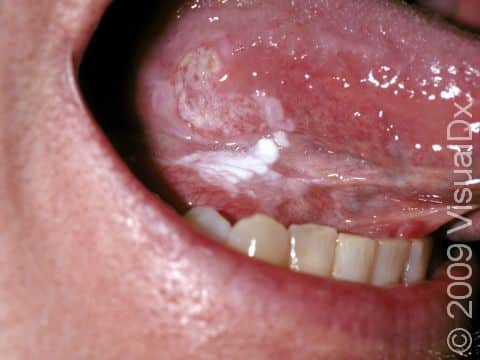
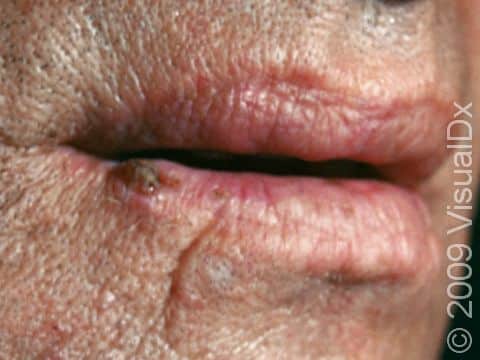
- Lower lip, especially in smokers.
In darker skin colors, the most common locations for SCC include the:
- Legs.
- Non-sun-exposed sites.
- Sites of chronic scarring.
- Non-healed leg ulcers.
- The genital and anal regions.
Self-Care Guidelines
Preventing sun damage is crucial to avoiding the development of SCC and other skin cancers:
- Avoid UV exposure from natural sunlight and from artificial tanning devices.
- Wear broad-spectrum sunscreens (blocking both UVA and UVB) with sun protection factor (SPF) 30 or higher, reapplying frequently.
- Wear wide-brimmed hats, sunglasses, and long-sleeved shirts. Some manufacturers make specialty clothing with an ultraviolet protection factor (UPF) rating.
- Avoid the sun when it is the strongest (between 10:00 AM and 3:00 PM).
Once a month, you should perform a self-exam to look for signs of skin cancer. It is best to perform the exam in a well-lit area after a shower or bath. Use a full-length mirror with the added assistance of a hand mirror. Using a hair dryer can help you examine any areas of skin covered by hair, such as your scalp.
- In front of a full-length mirror, inspect the front of your body, making sure to look at the front of your neck, chest (including under breasts), legs, and genital areas.
- With your arms raised, inspect both sides of your body, making sure to examine your underarms.
- With your elbows bent, examine the front and back of your arms as well as your elbows, hands, fingers, the areas between your fingers, and your fingernails.
- Inspect the tops and bottoms of your feet, the areas between your toes, and your toenails.
- With your back to the mirror and holding a hand mirror, inspect the back of your body, including the back of your neck, shoulders, legs, and buttocks.
- Using a hand mirror, examine your scalp and face.
As you perform your monthly self-exam, familiarize yourself with the moles, freckles, and other marks on your body, and look for any changes in them from month to month, including changes in shape, size, color, and other changes, such as moles that bleed or itch.
Treatments
If your medical professional suspects SCC, they will first want to confirm the diagnosis by performing a biopsy of the lesion. The procedure involves:
- Numbing the skin with an injectable anesthetic.
- Sampling a small piece of skin.
- Having the skin sample examined under the microscope by a dermatopathologist.
SCC treatment depends on a variety of factors, including the type and size of the cancer, location on the body, and microscopic features described in the biopsy report.
Mohs surgery is considered the most effective treatment for SCC, particularly on areas of the body that are cosmetically sensitive. It is also best for SCCs that may be higher risk due to type or size, or because they occur on a body location where SCCs are more likely to recur. In this technique, the physician takes tiny slivers of skin from the cancer site until the skin cancer is completely removed.
Surgical excision is another treatment that is used for SCCs in lower risk areas.
Radiation may also be recommended, as may oral anticancer therapies if the SCC is advanced.
Visit Urgency
If you have developed a new lesion on sun-exposed skin or if you have a spot that bleeds easily or does not seem to be healing, then you should make an appointment with a medical professional such as a dermatologist. You should also make an appointment if an existing spot on the skin changes size, shape, color, or texture, or if it starts to itch, bleed, or become tender.
Be sure to tell your medical professional when you first noticed the lesion and what symptoms there are (such as easy bleeding or itching). Also be sure to ask your family members if they have ever been diagnosed with skin cancer, and relay this information to your medical professional.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 26th, 2024 at 12:30 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder