Hives (Urticaria)
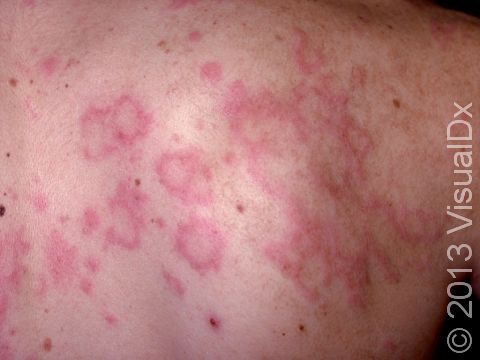
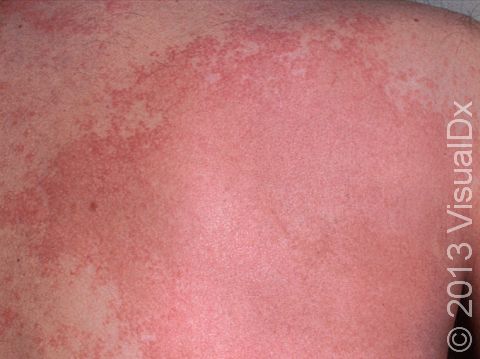
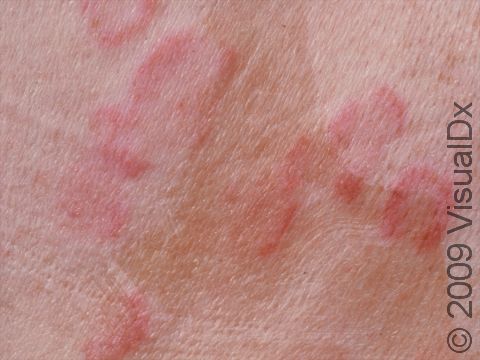
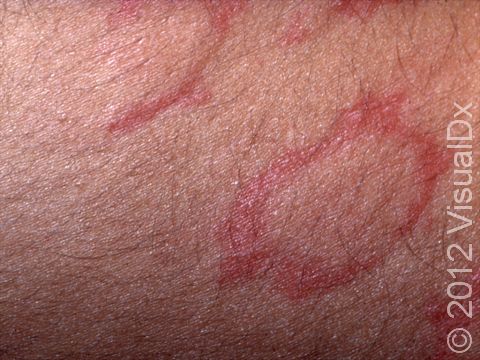
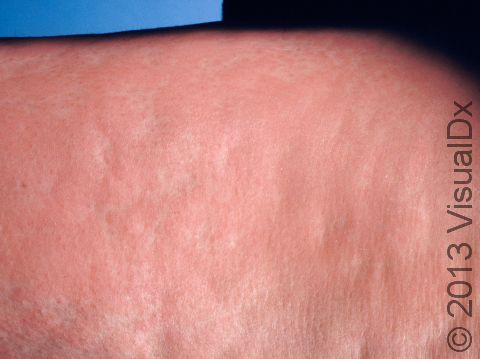
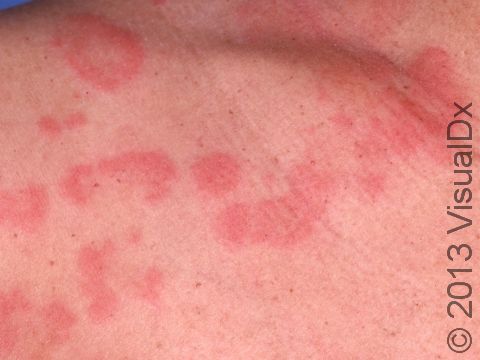
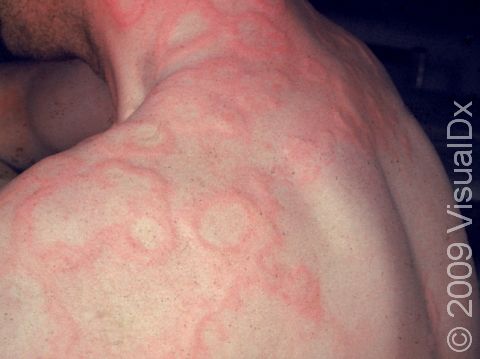
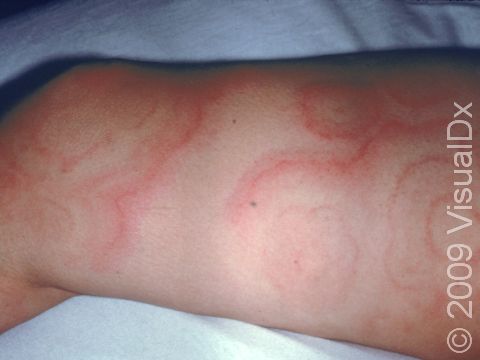
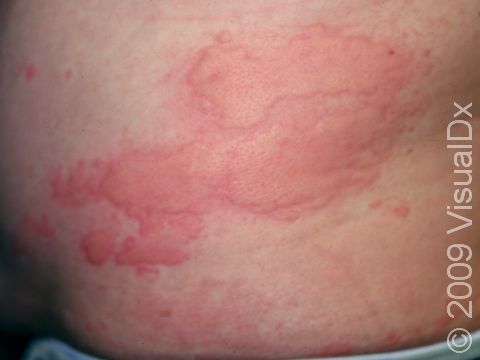
Hives (urticaria), also known as welts, is a common skin condition with an itchy rash of pink or red bumps (papules) that appears and disappears anywhere on the body. In darker skin colors, the redness may be harder to see, but the swollen skin bumps can be felt by the touch. An individual hive typically lasts a few hours (up to 24 hours) before fading away, and new hives can appear as older areas disappear.
Hives can be considered acute (new or periodic episodes lasting less than 6 weeks) or chronic (periodic episodes lasting more than 6 weeks). Although many people have a single episode of acute hives that goes away within a few days to weeks, some individuals may have chronic hives that persist intermittently for years.
Hives can be caused by many triggers, including:
- Medications, especially aspirin, ibuprofen, naproxen, narcotic painkillers, and antibiotics.
- Infections with viruses, bacteria, and fungi.
- Environmental allergies such as insect bites, pollen, mold, and animal dander.
- Physical exposures such as heat, cold, water, sunlight, and pressure.
- Medical conditions such as some blood diseases and cancer.
- Food allergies such as to strawberries, eggs, nuts, and shellfish.
In many cases, the causative trigger is not identified, despite extensive testing. This is referred to as idiopathic urticaria. In approximately 50% of idiopathic urticaria outbreaks, hives are most likely caused by a reaction from the person’s own immune system (autoimmune reaction).
Who's At Risk?
Hives appear in people of any age, race / ethnicity, and sex. Hives are very common; it is estimated that up to 20% of the population develops them at some point in their lives. Individuals with a family or personal history of atopic conditions (asthma, hay fever, eczema) are more prone to developing hives.
Acute hives are most common in children and young adults, and chronic hives are more often seen in females, especially middle-aged women.
Signs & Symptoms
The most common locations for hives include the:
- Trunk.
- Upper arms or upper legs.
- Hands and feet.
- Face.
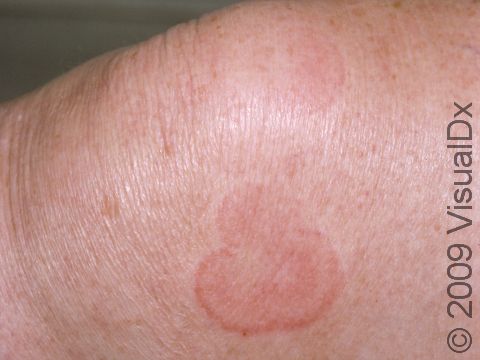
An individual hive appears as a well-defined pink or red swelling, which, in darker skin colors, may be easier to feel than see. The bumps range in size from 2 mm to over 30 cm. Some lesions may develop a lighter center. Hives usually appear in groups or batches. They are often incredibly itchy. Individual hives disappear within 24 hours, but a single episode with the development of new lesions may last much longer.
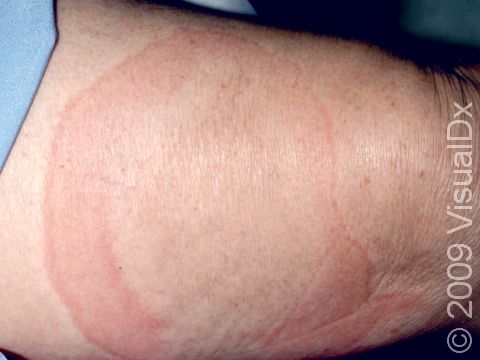
Dermographism is a type of urticarial reaction that appears within a few minutes of scratching the skin. The rash is usually seen in a straight line (linear) pattern. This is typically a sign of a person with sensitive skin.
Swelling of the eyes, mouth, hands, feet, or genitals can sometimes occur with hives. This swelling, called angioedema, usually goes away within 24 hours, but it can be quite severe and life-threatening when swelling of the airway occurs.
Hives are usually itchy, but they can also burn or sting.
Self-Care Guidelines
If you are experiencing mild hives, you can try:
- Taking cool showers.
- Applying cool compresses.
- Wearing loose-fitting clothes.
- Avoiding strenuous activity.
- Using an over-the-counter antihistamine such as cetirizine (Zyrtec), fexofenadine (Allegra), loratadine (Claritin), or diphenhydramine (Benadryl).
In addition, try to discover what is triggering your hives and avoid whatever it might be. In particular, consider any new foods that were ingested or new medications that were started.
Treatments
After confirming that you have hives, the medical professional will work with you to discover the possible cause. They will also take a detailed medical history and may do blood work, urine tests, or x-rays.
The best treatment for hives is to discover any triggers and stop your exposure to them. However, most people with hives do not know the cause and require medications to get rid of them.
The most common medications for hives include:
- Non-sleep-causing (nonsedating) antihistamines such as loratadine (Claritin), fexofenadine (Allegra), desloratadine (Clarinex, Aerius), or cetirizine (Zyrtec).
- Sleep-causing (sedating) antihistamines such as diphenhydramine (Benadryl), hydroxyzine (Vistaril, Atarax), or doxepin (Sinequan, Adapin, Zonalon).
- Other antihistamines such as cimetidine (Tagamet) or famotidine (Pepcid).
- Montelukast (Singulair), zafirlukast (Accolate), or zileuton (Zyflo).
In rare instances, your medical professional might prescribe oral corticosteroid pills (a steroid). Other classes of oral or injectable medications may be prescribed for recurrent hives that do not respond to these measures.
Visit Urgency
Call 911 if you are feeling lightheaded or are having difficulty breathing or swallowing associated with your hives.
In nonurgent situations with hives, see a medical professional if the hives do not improve with treatment or if they continue to appear for more than a few days.
Before visiting the medical professional, try to pay attention to what might be triggering your hives and whether it improves or worsens with exposure to heat, cold, pressure, or vibration. Take a list of every medication (prescription and over the counter), supplement, and herbal remedy you may have taken recently. Also consider any recent illnesses you may have had because some illnesses (and their treatments) can trigger hives.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 13th, 2024 at 11:58 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder