Mole, Atypical (Atypical Nevus)
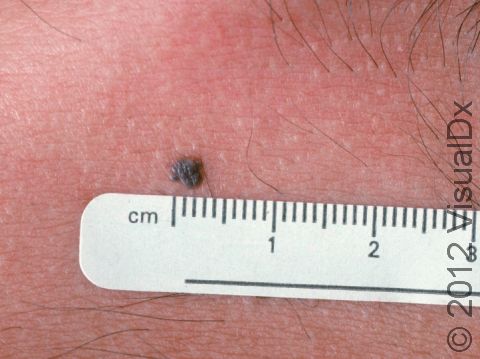
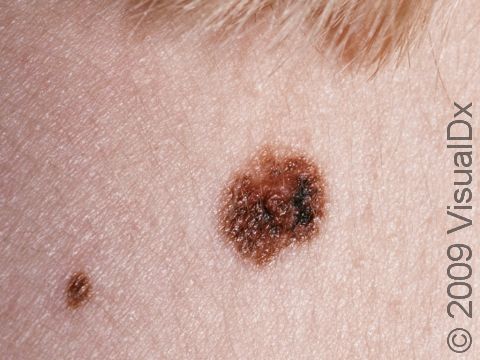
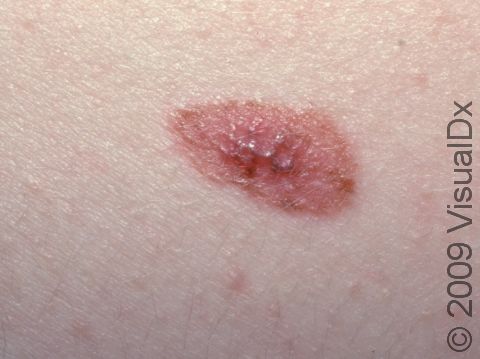
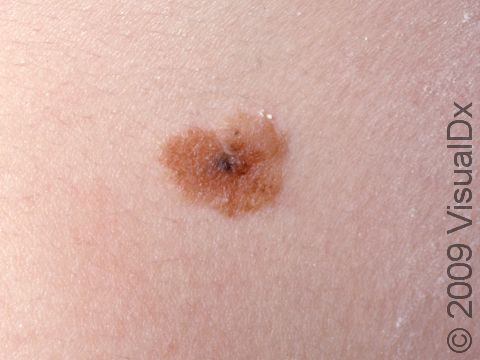
Nevus is the medical name for a mole. Moles (nevi) in which the skin cells are growing unusually are called atypical, or dysplastic, nevi. These moles are noncancerous (benign), despite their unusual appearance. All moles are made up of collections of the pigment-producing cells of the skin; they may be flat, raised, skin-colored, and pinker or darker than the surrounding skin. Atypical moles may have one or more of the ABCD criteria of the ABCDEs of skin cancer (melanoma), even though they are not cancerous:
- A – Asymmetry: One half of the lesion does not mirror the other half.
- B – Border: The borders are irregular or vague (indistinct).
- C – Color: More than one color may be noted within the mole.
- D – Diameter: Size greater than 6 mm (roughly the size of a pencil eraser) may be concerning.
- (And E – Evolving: Notable changes in the lesion over time are suspicious signs for skin cancer.)
Who's At Risk?
- Atypical moles may occur in any age, race / ethnicity, and sex.
- Atypical moles frequently run in families.
- People with atypical moles may also have a family history of melanoma.
Signs & Symptoms
- Atypical moles may appear anywhere on the skin. The lesions can vary in size and color.
- Atypical moles can be larger than a pencil eraser (6 mm) and may have variations in color within the lesion, ranging from pink to reddish-brown to dark brown.
- Atypical moles may be darker brown in the center or on the edges.
- People with atypical nevus syndrome may have hundreds of moles of varying sizes and colors.
Self-Care Guidelines
- If you suspect your child has an atypical mole, you should visit a dermatologist’s office to ensure it is not a melanoma.
- Protective measures, such as avoiding skin exposure to sunlight during peak sun hours (10 AM to 3 PM), wearing protective clothing, and applying high sun protection factor (SPF) sunscreen are essential for reducing exposure to harmful ultraviolet (UV) light.
- Monthly self-examination of your child’s skin is helpful to detect new lesions or changes in existing lesions.
Treatments
Biopsy or surgical removal (excision) may be done so the mole can be examined by a specialist (pathologist) to determine the exact diagnosis. This procedure may be performed by a dermatologist, plastic surgeon, or other type of surgeon.
People with multiple moles and atypical moles should be followed regularly by a dermatologist. At the dermatologist’s office, they may use whole-body photography or photographs of individual moles to follow such people.
Visit Urgency
- Seek medical evaluation for any mole with any of the ABCDE criteria to ensure it is not cancerous.
- People with multiple moles and unusual (atypical) moles should be examined at a dermatologist’s office every 4-12 months depending on their personal history and family history.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 26th, 2024 at 11:54 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder