Birthmark (Congenital Melanocytic Nevus)
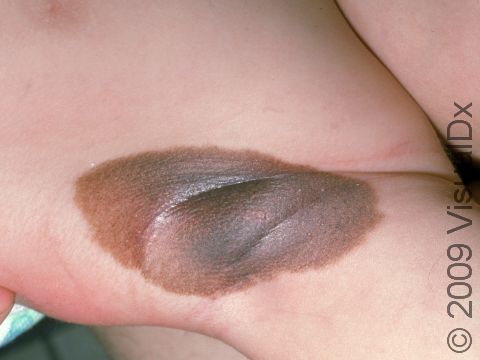
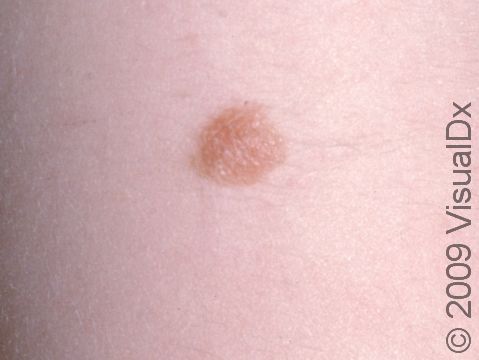
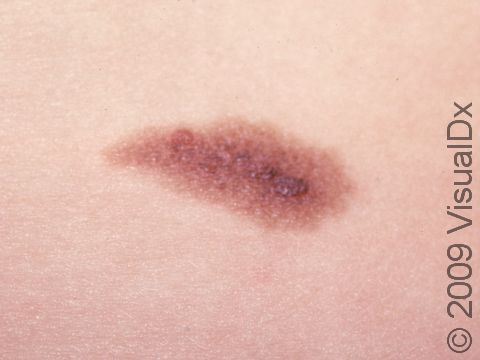
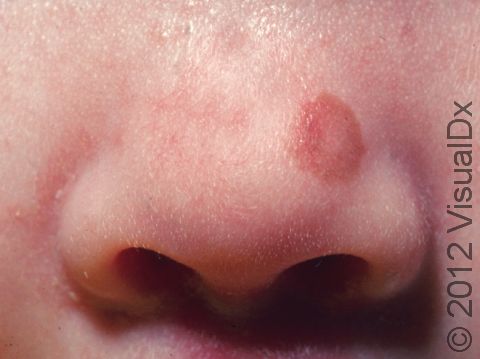
A congenital melanocytic nevus is a mole that is present at birth or shortly thereafter. It is one common type of birthmark. It is caused by a cluster of pigment-producing cells in the skin and sometimes in deeper tissues.
Congenital melanocytic nevus has a very low (2%-5%) lifetime risk of turning into a cancerous (malignant) mole called melanoma. This risk is higher in people who have large or giant (larger than 20 cm, or about 8 inches) congenital melanocytic nevi.
Large moles on the head or spine may have associated nervous system problems, although this is rare.
Who's At Risk?
Most people are born without moles but will gradually acquire them with age and sun exposure. Congenital means “born with,” so this type of birthmark is usually seen in babies, but they persist in people for life. Congenital melanocytic nevi are slightly more common in females than males.
Signs & Symptoms
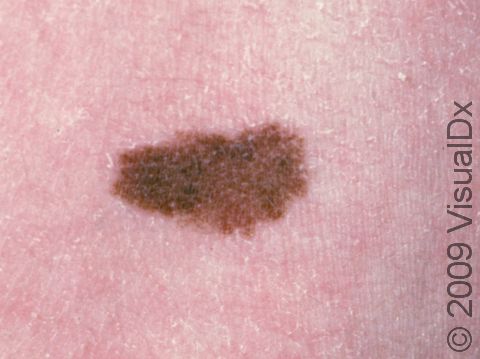
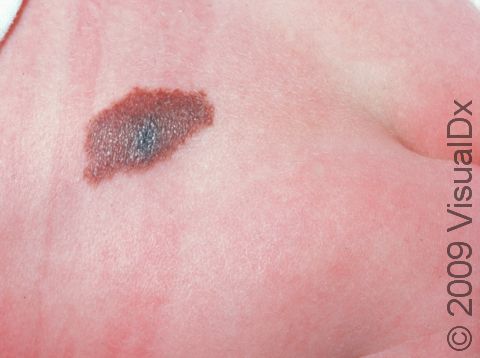
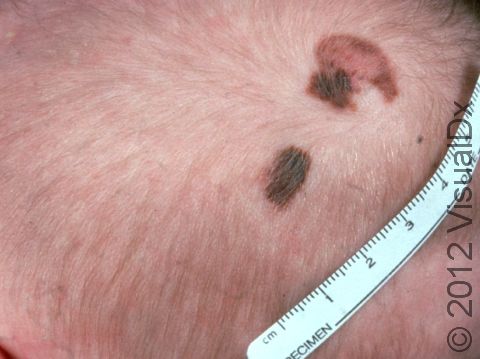
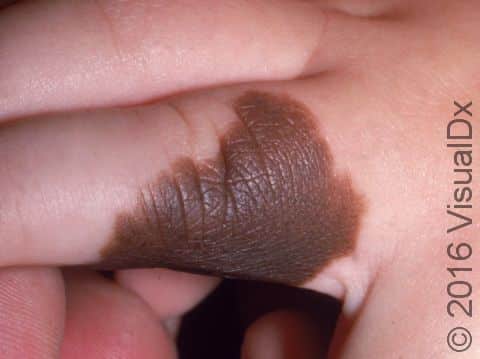
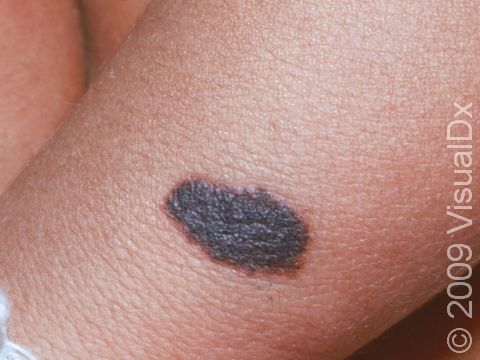
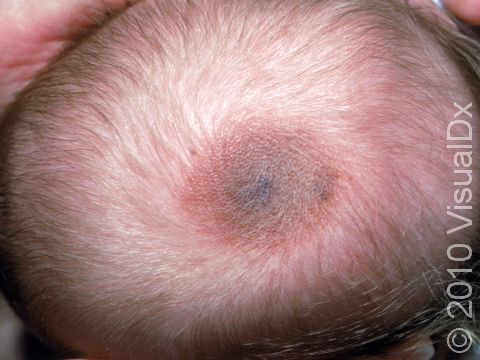
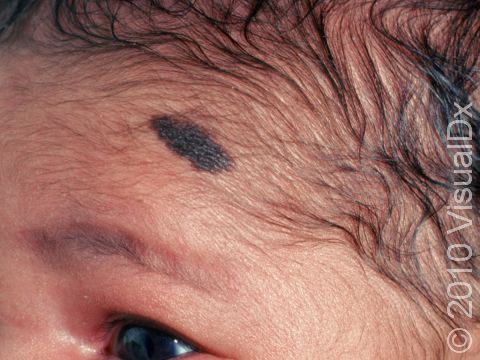
Congenital melanocytic nevi are brown or sometimes blackish papules (small, solid bumps) or patches (flat areas larger than a thumbnail) that are present at birth or shortly after (before age 1 year). They may have a smooth, round border, or the border may be irregular. There is often just one congenital melanocytic nevus, but there can be multiple, and they range in size from 1 cm to 20 cm (sometimes covering large sections of the body). Smaller surrounding lesions, called satellite lesions, are sometimes present with large lesions.
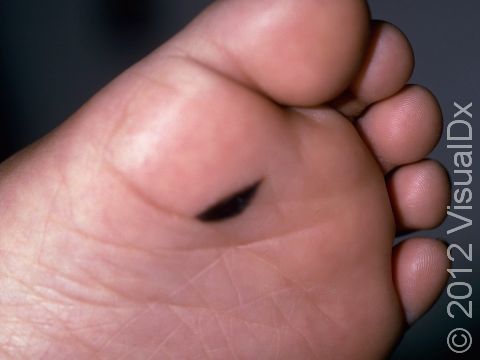
The most common locations for these birthmarks are the buttocks, thighs, and trunk, but lesions may occur on the face and arms or legs. They occasionally occur on the palms, soles, and scalp.
Changes in thickness, color, and hair content in the congenital melanocytic nevus may occur in childhood and especially during adolescence. In later adult years, they may fade in color to a lighter brown.
Self-Care Guidelines
Because there is a risk of the congenital melanocytic nevus becoming malignant, wear sun-protection clothing and use sunscreen that blocks UVB and UVA rays (ie, broad spectrum) with SPF 30 or higher every day (after age 1 year).
Treatments
The medical professional may simply recommend observation, which means watching it lifelong for any change in size (other than slow growth with a child), shape, or color and for any change in the surface (eg, flat areas that become more raised), or a skin biopsy may be done to confirm that there are no suspicious cells in the birthmark.
Small-to-medium-size congenital melanocytic nevi are often watched rather than removed. In addition to observing the mole for any changes, photographs may be taken to document and follow potential changes in the mole.
For larger moles, consultation and management by a medical professional, such as a dermatologist, with further consultation with a plastic surgeon, may be necessary. If the moles are numerous or involve the head or spine, consultation with a neurologist may be suggested.
Visit Urgency
Anyone with a birthmark should have it checked by a medical professional.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on July 10th, 2025 at 2:45 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder