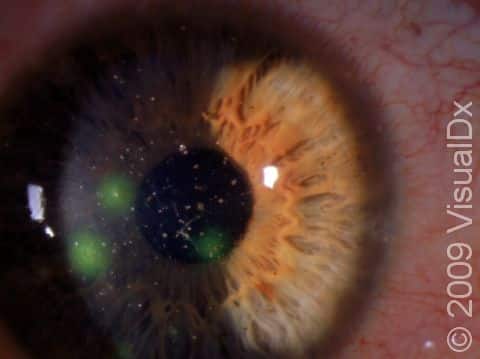
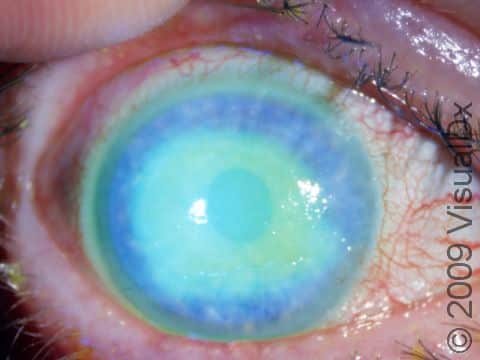
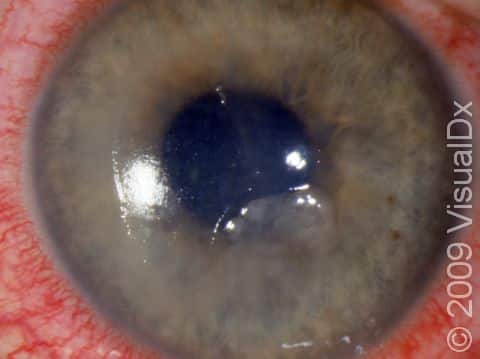
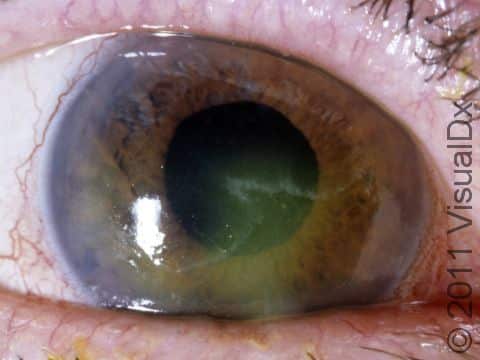
Corneal Abrasion
A corneal abrasion is a scratch or cut of the clear outer layer (cornea) of the eye. An injury is the most common cause of a corneal abrasion. The most common injuries to the cornea are:
- Scratches from fingernails (human and animal).
- Foreign objects touching the cornea (eg, dirt, wood splinters, metal shavings, plants, tree branches).
- Excessive rubbing of the eye.
- Overwearing of contact lenses, such as wearing them overnight.
- Wearing contacts that have not been cleaned properly.
- Wearing ill-fitting contact lenses.
- Wearing torn contact lenses.
- Makeup brushes.
- Eyelashes rubbing the cornea.
- Foreign objects that get caught under the eyelid, irritating the cornea when you blink.
Who's At Risk?
Corneal abrasions are fairly common. People who wear contact lenses or live or work in dusty, dirty, windy, or debris-laden areas are more likely to get a corneal abrasion.
Signs & Symptoms
It is very difficult to see a corneal abrasion with the naked eye. However, you may have a corneal abrasion if you have experienced any of the causes of trauma mentioned above along with an unrelenting painful, gritty feeling in your eye. You may also experience:
- Lots of watery tearing.
- Sensitivity to light (especially bright light).
- Blurry vision.
- Redness of the eye.
Self-Care Guidelines
If you have the signs and symptoms of a corneal abrasion, you can try:
- Sitting in a dark room and keeping your eyes shut.
- Not rubbing or pressing on the injured eye.
- Immediately removing contact lenses, if applicable.
- Using clean water to rinse the eye and wash out any foreign objects.
- Wearing sunglasses to reduce light sensitivity.
There are precautions you can take to prevent getting a corneal abrasion. These include:
- Wearing protective eyewear for all conditions that may result in a corneal abrasion, such as working in the garden, working on grinding machines, etc.
- Being extra careful when using makeup brushes.
- Taking good care of and using excellent hygiene with contact lenses.
- Never sleeping in contact lenses, regardless of manufacturer notes.
- Keeping your nails cut short.
Note: If the corneal abrasion heals and then suddenly recurs days later, this may be a sign of recurrent corneal erosion, which requires specific medical care by an eye care professional. Use of topical anesthetic solutions is only for the short term. Using these drops more than once or twice is dangerous because it slows healing and could lead to more serious conditions.
Treatments
Your medical professional will examine the eye and check for any foreign objects and, if needed, clean the area. Numbing eye drops or oral pain medication may be given. Topical antibiotics also may be used. If the abrasion was contact-lens-related, a reevaluation of your contact lens fit and type may be required.
Visit Urgency
See a medical professional if you have:
- Persistent eye pain that is increasing despite self-care.
- Had a piece of metal, wood, or plant material hit the eye with high speed that may have penetrated the eye, not just irritated it.
- Any abrasion caused by chemicals, heat burn, makeup brushes, or plant materials.
- Suspected that a foreign object is stuck in your eye.
- Recurrence of the pain and other symptoms days after an initial eye injury.
- Mucus or pus-like discharge from the eye.
- Progressive vision loss.
Trusted Links
References
Boyd K. Corneal abrasion and erosion. American Academy of Ophthalmology. https://www.aao.org/eye-health/diseases/what-is-corneal-abrasion. 2023 Oct 23.
Hayden, Jr J, Chumley HS. Corneal foreign body and corneal abrasion. In: Usatine RP, Smith MA, Mayeaux EJ, Chumley HS, eds. The Color Atlas and Synopsis of Family Medicine. 3rd ed. New York, NY: McGraw-Hill Education; 2019.
Knoop KJ, Palma JK. Corneal abrasion. In: Knoop KJ, Stack LB, Storrow AB, Thurman R, eds. The Atlas of Emergency Medicine. 5th ed. McGraw-Hill; 2020.
Last modified on June 20th, 2024 at 7:28 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder