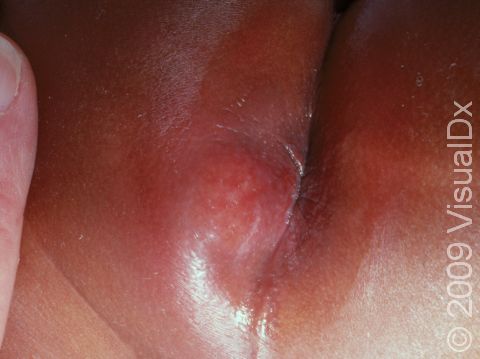
Abscess
An abscess is an infection characterized by a collection of pus under the skin. Bacteria commonly causing abscesses are Staphylococcus aureus (commonly known as “staph”) and Streptococcus (commonly known as “strep”). These bacteria enter the skin through any cracks or injury to the skin. The area of skin then becomes tender, warm, and swollen over days to 1-2 weeks, and a fever may develop. Abscesses can sometimes form if minor superficial skin infections are not treated appropriately and in a timely fashion. Most abscesses resolve quickly once appropriately treated.
Who's At Risk?
Abscesses may occur at any age, including in infants.
Signs & Symptoms
A worsening tender swelling that arises over a period of 1-2 weeks. In lighter skin colors, abscesses may appear red or purple, and in darker skin colors, they may appear purple or brown. The pus underneath the skin is usually not visible, but you may be able to feel fluid in the abscess when you press on it. The baby may have a fever or seem generally unwell.
Self-Care Guidelines
There are no self-care options for abscesses. While waiting to see your baby’s medical professional, you can try applying a warm compress to the affected area and giving them ibuprofen (eg, Advil, Motrin; in infants older than 6 months) to help with the swelling and pain.
To prevent the spread of infection to others, infected wounds, hands, and other exposed body areas should be kept clean, and wounds should be covered until healed.
Treatments
Your baby’s medical provider may drain the pus or fluid collection by making a small incision in the skin after it has been numbed. This will drain most of the bacteria, helping the body fight the small amount of bacteria that remains. This fluid may then be sent to a laboratory for testing (a bacterial culture). The culture can determine what type of bacterium is causing the infection and also what antibiotics will work best to treat it. The medical professional may choose to have your baby start oral antibiotics aimed at treating the most common bacteria that cause abscesses. However, if the infection is small and it has been drained, they may decide not to treat with oral antibiotics.
If your baby’s symptoms are not improving or it is determined that the bacterium is not one of the common types, the medical professional may prescribe different antibiotics. If antibiotics are prescribed, it is important for your baby to take the entire course as prescribed, even if they are feeling better or the infection appears to be gone after just a few days. If your baby has been taking antibiotics and the infection has not improved or if they continue to seem unwell after about 2-3 days, return to see their medical professional.
Visit Urgency
A worsening tender swelling should prompt you to make an appointment with your baby’s medical provider as soon as possible. If the area involves the face, spreads very rapidly, or is in an area that severely limits their functionality, you should seek emergency care for the baby.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 14th, 2024 at 1:33 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder