Thrush (Oral Candidiasis)
Oral candidiasis, commonly known as thrush, is a yeast infection of the mouth or throat. The yeast that most commonly causes oral candidiasis is Candida albicans.
Who's At Risk?
Thrush is most common in babies, but it can also occur in children and adults.
Children who develop thrush most commonly include those:
- With diabetes or other glandular (endocrine) disorders.
- With genetic disorders such as Down syndrome.
- Who are taking oral antibiotics.
- Undergoing chemotherapy.
- With leukemia or lymphoma.
- With poor nutrition.
- With an immune deficiency, such as HIV.
- Using inhaled steroids for certain lung conditions.
- With cavities or poor dental hygiene.
Signs & Symptoms
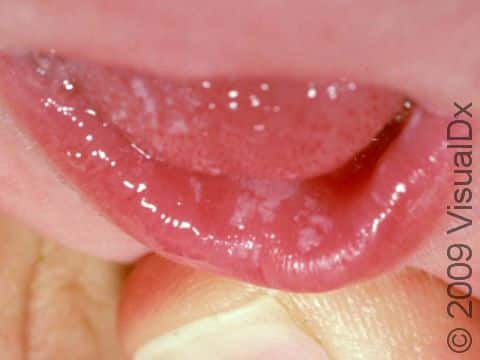
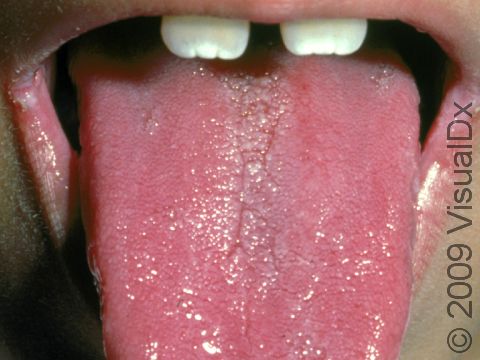
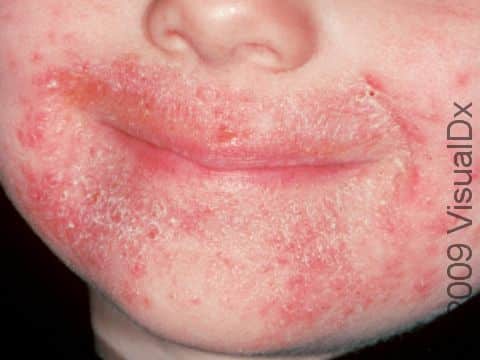
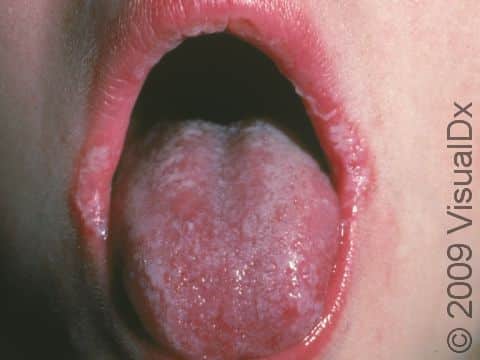
Thrush may appear as white or pale-yellow papules (raised, solid bumps) or plaques (flat, solid areas) on the inner surfaces of the mouth and throat, the tongue, and the lips. It may resemble cottage cheese or milk curds. Scraping off these membranes may be difficult and may leave slightly bleeding sores. Thrush can sometimes appear as red, sore areas.
Thrush may be accompanied by a burning sensation in the mouth or throat.
Self-Care Guidelines
Thrush may make eating and drinking uncomfortable, and children with thrush may become dehydrated as a result. For this reason, it is important to make sure your child maintains good nutrition and fluid intake while infected with thrush.
Good oral and dental hygiene are important measures in treating and preventing thrush, so be sure your child brushes their teeth and tongue every morning and night, and ideally after every meal.
Treatments
It is important to seek medical treatment that will help kill the overgrown yeast. Your child’s medical provider can prescribe an antifungal medication such as:
- Nystatin – Nystatin comes in a suspension or liquid, and also in a lozenge, called a troche. Have your child swish the suspension around the mouth and then swallow it. The lozenge dissolves in the mouth. Use the suspension and/or lozenges several times a day until the lesions are completely gone.
- Amphotericin B suspension – Swish the suspension around in the mouth and swallow it several times a day until the lesions are completely gone.
- Fluconazole pills or a suspension – Swallow this medication once daily for 5-10 days.
Visit Urgency
Thrush requires prescription medication, which your child’s medical professional can prescribe after an evaluation. If your child has an immune system deficiency, it is particularly important that they receive prompt treatment to keep the yeast out of the bloodstream and prevent it from infecting other parts of the body.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 17th, 2024 at 9:43 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder