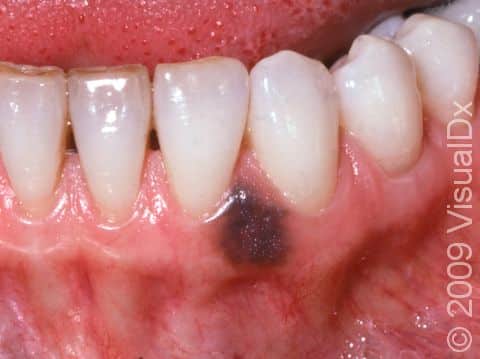
Oral Melanotic Macule
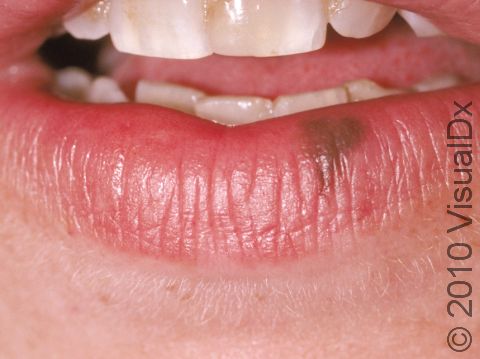
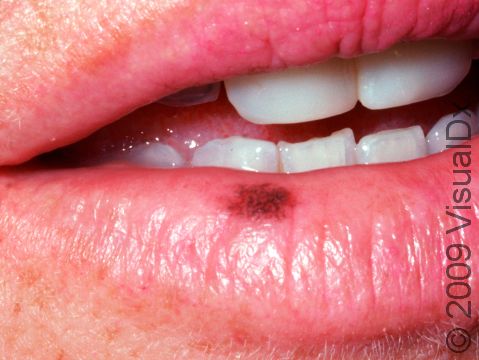
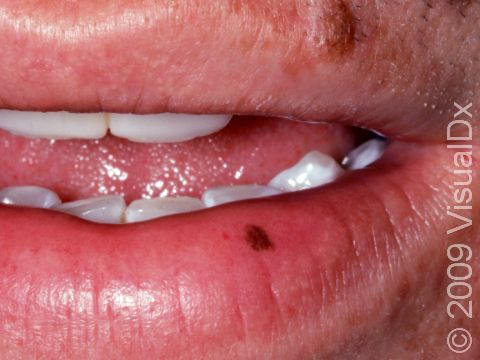
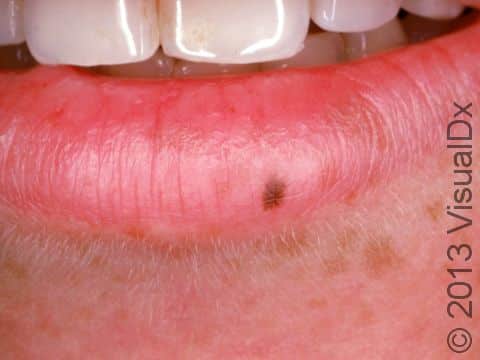
An oral melanotic macule is a harmless dark spot found on the lip, most often the lower lip, or inside the mouth, either on the gums, inside the cheek, or on the roof of the mouth. An oral melanotic macule found on the lip is sometimes called a labial melanotic macule.
Who's At Risk?
Oral melanotic macules can appear in people of any age, race / ethnicity, and sex. However, they are more common in middle-aged individuals, people with darker skin colors, and in females.
Signs & Symptoms
The most common locations for an oral melanotic macule include the:
- Lips, especially the lower lip.
- Gums (gingiva).
- Inner cheek (buccal mucosa).
- Roof of the mouth (hard or soft palate).
An oral melanotic macule appears as a brown or grayish-brown macule (a small flat, smooth area of skin or mucosa) usually less than 7 mm in diameter. It has a well-defined border and a uniform color.
People can have more than one oral melanotic macule.
Self-Care Guidelines
There are no self-care measures for oral melanotic macules.
Treatments
If the diagnosis of oral melanotic macule is not certain, your medical professional may perform a biopsy to confirm the diagnosis. The biopsy can help determine whether the lesion is a benign oral melanotic macule or a malignant melanoma, a type of skin cancer.
Most dark lesions on the lips or inside the mouth are harmless oral melanotic macules. Usually, your medical professional will simply want to observe the lesion by measuring it, taking a photograph of it, or both. As long as the oral melanotic macule stays stable in size, shape, and color, no treatment is needed.
If you would like a labial melanotic macule removed for cosmetic reasons, your medical professional may recommend laser treatment.
Visit Urgency
See your medical professional for any new dark lesion on the lips or inside the mouth. Similarly, any existing lesion that changes size, shape, or color should be evaluated promptly.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 24th, 2024 at 11:06 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder