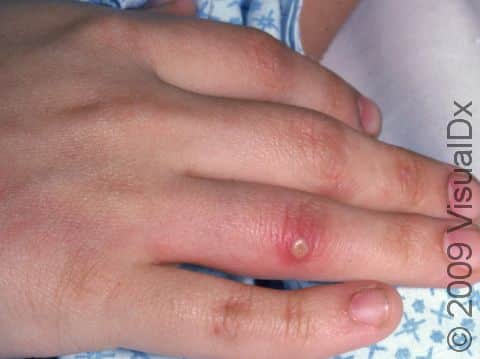
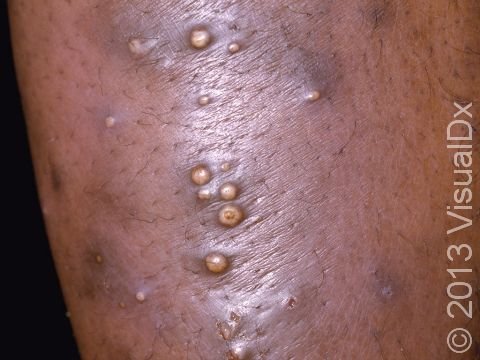
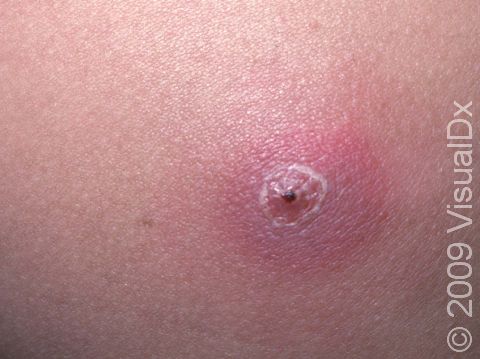
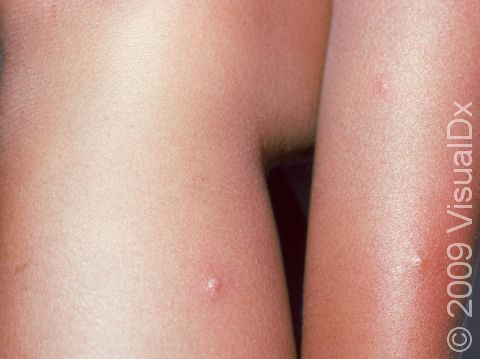
Boils (Furunculosis)
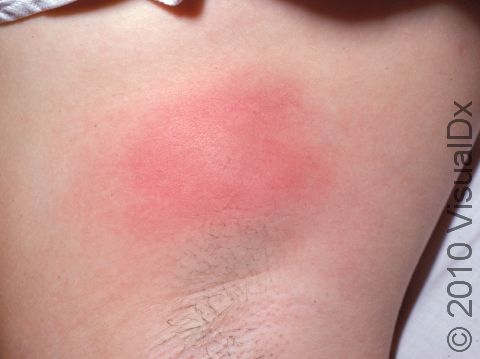
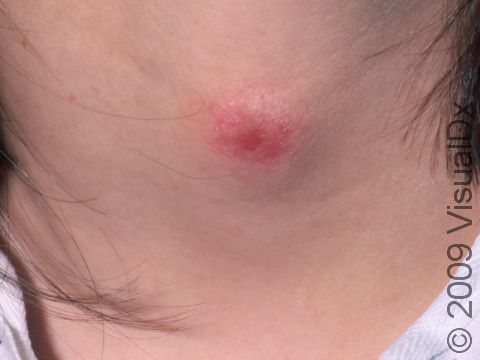
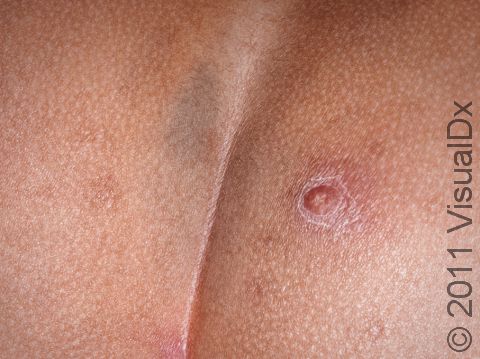
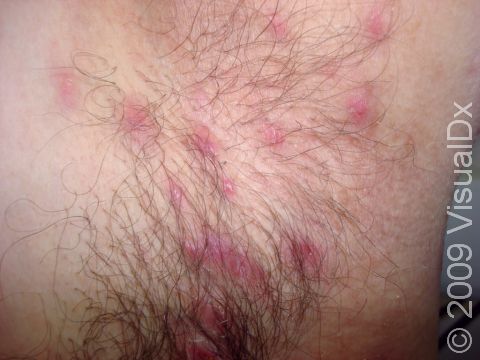
Boils (furuncles) are painful pus-filled bumps (pustules) on the skin resulting from the deep infection of a hair follicle. The infection is usually caused by a type of bacteria called Staphylococcus aureus (commonly known as “staph”). Many people are carriers of staph bacteria, meaning that it normally lives on their skin or in their nose without doing them any harm. Tiny breaks in the surface of the skin (such as those caused by friction or scratching), however, can help the bacteria gain entry into and infect the hair follicle, resulting in a boil.
Boils may resolve with simple self-care measures, but the pus needs to drain in order for them to heal completely. Many boils eventually drain on their own, or they can be drained by a medical professional. Antibiotics may also be prescribed. Untreated boils can enlarge or grow together to form a giant multi-headed boil called a carbuncle. Rarely, the infection in the skin can get into the bloodstream, leading to serious illness.
Who's At Risk?
Boils are most common in teenagers and young adults, and they are more common in males than females.
People who are particularly prone to developing boils include:
- Athletes participating in contact sports or using shared equipment.
- Individuals with a weakened immune system, such as those with HIV, diabetics, and people taking certain medications such as those used to prevent rejection of a transplanted organ or to treat cancer (chemotherapy).
- Individuals with another skin condition that may lead to scratching or other injury to the skin (eg, eczema, scabies).
- Carriers of staph.
- People who are obese.
- Individuals with poor nutrition.
- People living in close quarters with others (eg, military barracks, prison, homeless shelters).
Signs & Symptoms
A boil is a tender lump on an area of the skin that also has hair. In lighter skin colors, boils may appear red or purple, and in darker skin colors, they may appear purple or brown. The most common areas for boils to occur are places where there is friction, such as the buttocks, armpits, groin, neck, shoulders, and face. The skin surrounding the boil may look swollen and red or purplish. The center of the boil eventually becomes filled with yellow or white pus that you can see just under the skin’s surface.
Self-Care Guidelines
Warm compresses applied to the area for 20 minutes at least 3-4 times a day may ease the discomfort and help encourage the boil to drain. If the boil starts to drain, wash the area with antibacterial soap and apply some triple antibiotic ointment and a loose bandage. Repeat this process of cleansing and bandaging the area 2-3 times a day until the skin has healed.
Boils can be very contagious. Do not share clothing, towels, bedding, or sporting equipment with others while you have a boil. Wash your hands frequently with antibacterial hand soap to avoid spreading the infection to others.
Use an antibacterial soap on boil-prone areas when showering, and dry your skin thoroughly after bathing. Avoid tight-fitting clothing and activities that cause a great deal of sweating.
Do not pop the boil yourself, such as with a pin or needle. Doing so may make the infection worse.
Treatments
The pus inside of a boil needs to be drained thoroughly before the body can completely clear the infection. If the boil does not drain with self-care measures, your medical professional may perform a simple procedure where a sterile needle or small blade is used to “nick” the skin over the top of the boil and the pus drains out. The area will then be cleaned and bandaged, and you will be instructed to wash, apply antibacterial ointment, and re-bandage the area several times daily. You may also be prescribed oral antibiotics.
Your medical professional may collect a swab of the pus for laboratory analysis and swabs from other areas of the body (eg, nose, armpits, and/or anus and genital area) to determine if you are a carrier of staph. If you are a carrier, you may be prescribed a topical medication applied to the inside of the nose and/or oral antibiotics for several days. These measures can help prevent a recurrence of boils and decrease the possibility that you may unknowingly spread the bacteria to others. If you are prescribed antibiotics, be sure to take the full course of treatment to avoid worsening of the infection and the development of bacterial resistance to the antibiotic.
Visit Urgency
See your medical professional if:
- You have multiple boils or if the boil(s) increases in size.
- You have a fever or chills, severe pain, or otherwise feel unwell.
- The boil fails to drain.
- The area of redness surrounding the boil begins spreading.
- You have diabetes, a heart murmur, a problem with your immune system, or are taking immune-suppressing medications when you develop a boil.
- You have had repeated outbreaks of boils.
If you are currently being treated for a skin infection that has not improved after 2-3 days of antibiotics, return to your medical professional.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 14th, 2024 at 1:45 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder