Juvenile Plantar Dermatosis
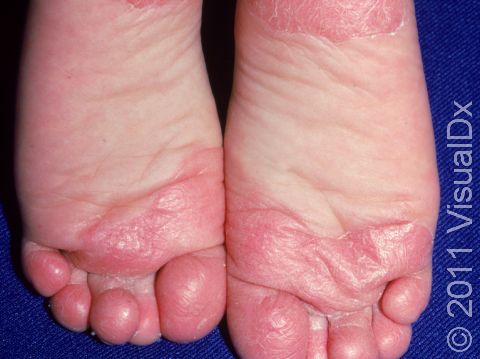
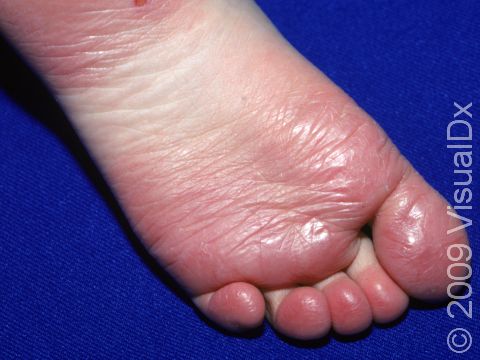
Juvenile plantar dermatosis, sometimes called sweaty sock syndrome, is a condition where the skin becomes scaly and sometimes cracked on the soles of the feet of children and young teenagers.
The cause of juvenile plantar dermatosis is unknown, but alternating moist / sweaty and dry conditions may lead to the condition. The condition tends to last, on average, about 3 years, usually going away once the child reaches puberty, but it may also continue during puberty.
Who's At Risk?
Juvenile plantar dermatosis occurs most often in children aged 3-15, but it is especially common in boys aged 4-8.
Children who have eczema (atopic dermatitis) seem to have a higher risk for developing juvenile plantar dermatosis.
Signs & Symptoms
Juvenile plantar dermatosis occurs as shiny, red patches on the weight-bearing surfaces of the feet. The skin appears tight and often smooth. Occasionally, painful cracks may be present. Even though children may complain of sweating, the skin feels dry and scaly.
The most common locations for juvenile plantar dermatosis include the:
- Big toe.
- Ball of the foot.
- Heel of the foot.
The creases between the toes (toe webs) are not usually affected.
Self-Care Guidelines
If you suspect your child has juvenile plantar dermatosis, have them:
- Try wearing sandals or breathable shoes. (Avoid shoes made from synthetic materials.)
- Avoid wearing shoes with rubber or plastic soles.
- Wear thick cotton socks and change them if they get sweaty or wet.
- Wash the feet daily using gentle, nonsoap cleansers (eg, Dove Sensitive Skin Beauty Bar).
- Apply petroleum jelly (eg, Vaseline) or thick moisturizers (eg, CeraVe Moisturizing Cream) to the feet at night.
- Apply barrier creams containing dimethicone during the day.
- Seal cracks in the skin with liquid bandage.
Treatments
The medical professional may first want to check your child for a fungal foot infection (eg, tinea pedis, or athlete’s foot) by scraping off a small amount of scale and examining it under a microscope. If fungus is not seen, it further suggests the diagnosis of juvenile plantar dermatosis.
Once the diagnosis of juvenile plantar dermatosis has been confirmed, the medical professional may recommend the following in addition to the self-care measures discussed previously:
- Prescription-strength topical corticosteroid (cortisone) cream or tacrolimus ointment
- Topical preparations that can remove scales, if very scaly, such as urea cream
- An oral antihistamine if itching is severe
- Treatments to help diminish sweating, such as aluminum chloride
Visit Urgency
See your child’s medical professional if they have red, scaly feet that have not improved with self-care measures. If the child has cracks in the skin in addition to a foot rash, try to see the medical professional even sooner.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 18th, 2024 at 1:34 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder