Diabetic Ulcer (Neurogenic Ulcer)
Neurogenic ulcers, also known as diabetic ulcers, are ulcers (areas of missing skin) that occur most commonly on the bottom of the foot. People with diabetes are predisposed to peripheral neuropathy, which means they have a decreased or total lack of sensation in the feet. Feet are naturally stressed from walking, and someone who has decreased sensation will not necessarily feel that they have an area of skin breakdown occurring. In addition to this lack or absence of sensation, there is a decrease in blood circulation to the feet. Wounds that do not get proper blood flow are not only slower to heal but are also at an increased risk for infection. A small cut, scrape, or irritated area in a person with diabetes can turn into an ulcer for these reasons. It is common for these types of ulcers to keep coming back in people with diabetes.
Who's At Risk?
Up to one-third of people with diabetes may be affected by neurogenic ulcers. The more serious or severe a person’s diabetes is and the more out of control or higher their blood sugar is, the more likely they are to develop ulcers. Other risk factors for developing neurogenic ulcers include obesity, heart disease, and tobacco use.
While neurogenic ulcers most often occur in people with diabetes, any condition resulting in peripheral neuropathy will predispose a person to developing a neurogenic ulcer.
Signs & Symptoms
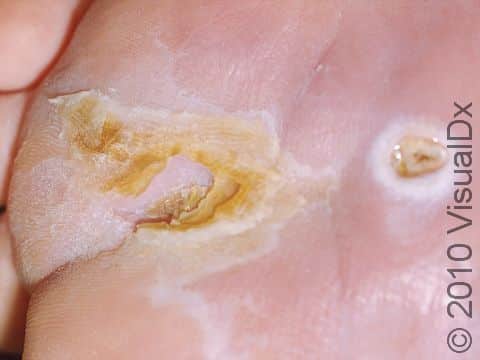
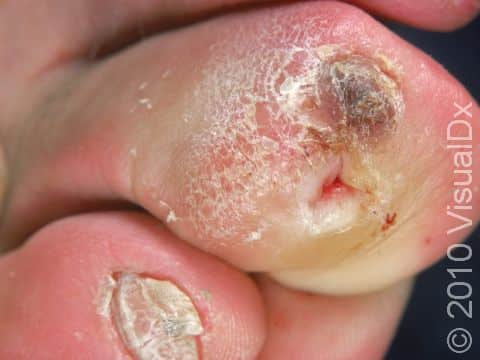
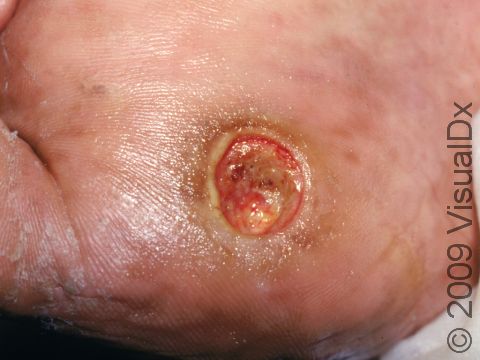
An ulcer is an open wound that can be deep enough that you can see to the bone. The ulcers are surrounded by a thick callus and may have a gray or black base. There may also be surrounding swelling and redness.
Diabetic foot ulcers commonly occur on the pressure points of the foot: the ball, heel, the tips of the toes, and side of the foot if a person’s shoes are too tight. However, an ulcer can form in any location that gets cut or scraped if it fails to heal properly.
Self-Care Guidelines
If you have had a neurogenic ulcer previously, it is common to get more. To help prevent neurogenic ulcers from forming:
- Inspect your feet daily, including the areas between the toes, to look for any breaks in the skin; blisters; or red, irritated areas. A mirror can help you see the bottoms of your feet, or have a family member or caregiver do this.
- Trim your toenails regularly.
- Make sure to wear well-fitting, cushioned shoes and pressure-reducing hosiery, both indoors and outdoors, to reduce risk of injury. If you wear socks, make sure any folds in the socks are smoothed out before putting shoes on. Avoid wearing flip-flops and wearing shoes without socks.
- Do not go barefoot; there is significantly more pressure on bare feet than feet in properly fitting, cushioned shoes.
- Do not use medicated pads to treat corns, calluses, or warts on the feet, as these pads can cause ulcers; instead, see a medical professional for removal.
- Test bath water with your fingers instead of stepping in it; if your feet lack sensation, they may get burned by water that is too hot.
- Try to decrease pressure on your feet by walking less (try nonweight-bearing exercise, such as swimming, cycling, or rowing) and, if applicable, consider changing to a job that does not require much walking or standing.
- Avoid smoking, as it can worsen blood flow, further slowing down healing.
- Control your blood sugar, as elevated blood glucose reduces the body’s ability to fight infection and slows down wound healing.
Treatments
In the case of a new ulcer, your medical professional may want to take an x-ray of the area to make sure there is no infection of the bone (osteomyelitis), fracture of the bone, or foreign objects lodged in the ulcer, as you may not feel them. Next, the medical professional will likely remove any dead tissue with a scalpel (a procedure called debridement) from the area, revealing healthy skin. While this will make the ulcer larger and cause bleeding, it is important to have healthy tissue exposed for faster and cleaner healing.
Your medical professional may send a sample of skin or fluid for bacterial culture and prescribe oral antibiotics if there is concern the skin is infected.
A variety of dressings or ointments may be recommended for wound care.
Your medical professional may have you wear a special cast to allow you to continue to be mobile but take pressure off the area. There are also medications that use growth factors to stimulate wound healing that your medical professional may prescribe.
It is very important to follow up with your medical professional as scheduled; neurogenic ulcers can worsen very quickly and need to be closely monitored. Make sure to call your medical professional if you experience any of the following: redness of the area, red streaking up the leg, drainage of the area, pain, foul odor, rising blood glucose, or swelling or redness of the top of the foot.
Visit Urgency
People can develop peripheral neuropathy without even being aware of it, so it is important for people with diabetes to be examined by their medical professional every 6 months; the medical professional can use a monofilament test to assess the sensation on the bottoms of your feet.
All ulcers should receive treatment. Also see your medical professional if you notice a lack of sensation in your feet or if there are any corns, calluses, or warts on the feet; skin discoloration, pain, swelling, or oozing of the feet; or if you have a fever.
Neurogenic ulcers can lead to amputation if care is delayed, so it is important to be seen by your medical professional as soon as possible.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on June 26th, 2024 at 4:44 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder