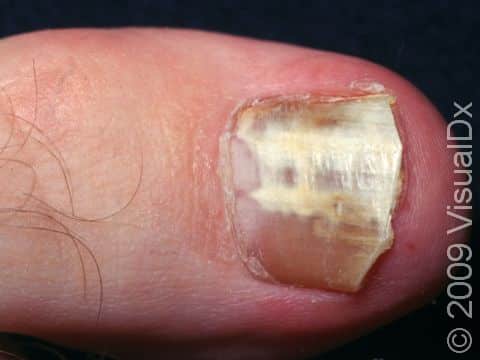
Nail Infection, Fungal (Onychomycosis)
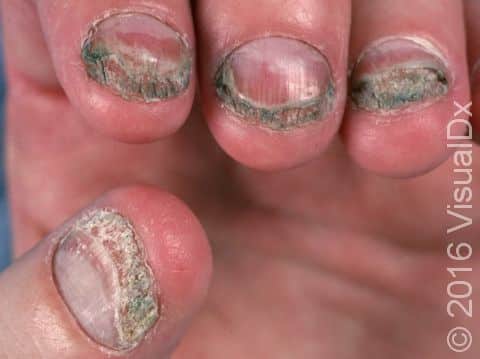
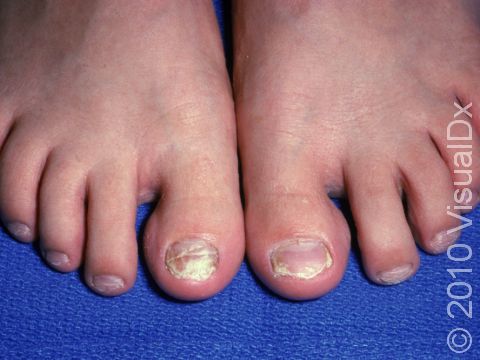
Onychomycosis, commonly known as a fungal nail infection, is an infection of fingernails and toenails by forms of fungi, mold, and yeast. Fungal nail infections are quite common and account for nearly half of all nail disorders. In the most common form of fungal nail infections, fungus grows under the nail and spreads along the nail bed and the grooves on the sides of the nails.
Who's At Risk?
Fungal nail infection may occur at any age but is more common in older adults. It is also more common in males. People with diabetes and certain other medical conditions may be more likely than others to develop a fungal nail infection. Other predisposing factors include being immunosuppressed or having eczema, psoriasis, or Down syndrome. Fungal nail infections are also more common in people who wear tight shoes habitually, those who are obese, and those with excessive sweating (hyperhidrosis).
Signs & Symptoms
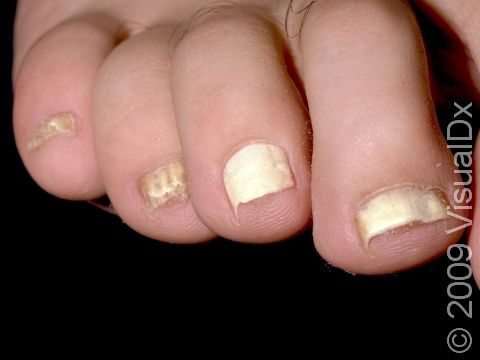
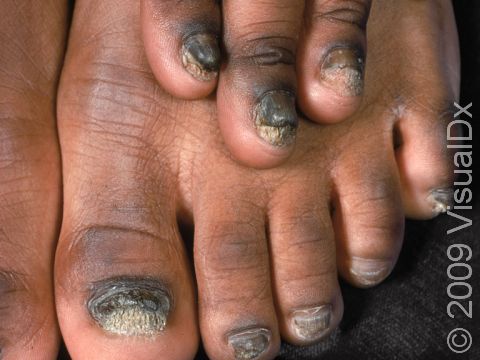
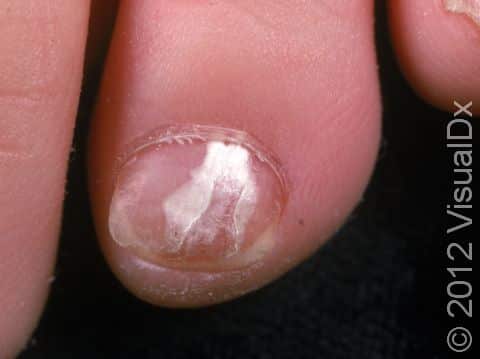
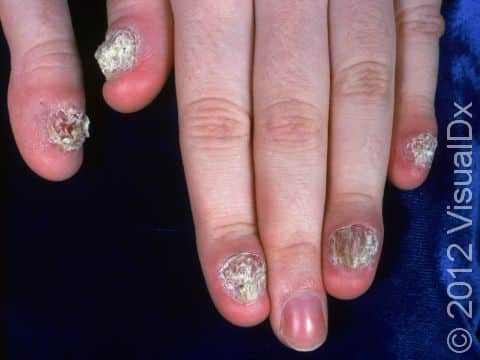
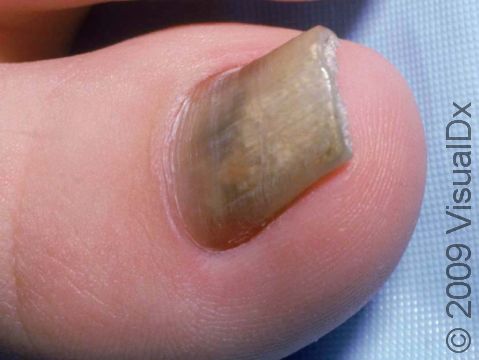
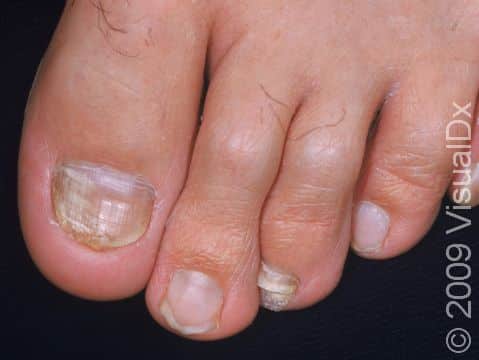
Fungal nail infection commonly starts as nail thickening, yellowish discoloration of the nail, and nail lifting from the nail bed (called onycholysis). When there is nail lifting, you may be able to see debris under the nails. The nails may eventually start to crumble, and you may lose the nail.
The toenails are most commonly affected by fungal nail infections. If the fingernails are affected, the toenails are usually affected as well. One, a few, or all nails may be affected.
Fungal nail infections sometimes occur along with athlete’s foot (tinea pedis) and/or oozing bacterial infection (paronychia), caused by inflammation and infection with yeast and/or bacteria in the region where the skin of the finger meets the base of the nail.
Self-Care Guidelines
To prevent spreading fungal nail infection to others and to avoid reinfection:
- Keep your nails clean and dry.
- Keep your nails short.
- Disinfect nail clippers after each use, and wash your hands after clipping infected nails.
- Avoid going to the nail salon.
- Do not apply nail polish or artificial nails to the infected nails.
If the toenails are affected:
- Wear socks and shoes that allow your feet to breathe. Consider throwing away old shoes or treating them with antifungal powder.
- Wear footwear in public areas such as public showers, pools, and locker rooms.
Over-the-counter products such as Kerasal nail patches or urea cream can help to thin out thick nails, but it may take months to see the effects.
If you also have athlete’s foot, treat that infection as well.
Treatments
Your medical professional may perform testing, such as by scraping or clipping the nail and looking for fungal growth under a microscope. They may also recommend seeing a podiatrist to cut back long or thick nails.
Depending on the severity of infection, your medical professional may prescribe:
- Topical therapy with ciclopirox nail lacquer or efinaconazole nail solution, which requires daily application for many months.
- Prescription-strength urea cream to thin out the nail, which also requires application for many months.
- Oral antifungal treatments offer the best chance for curing fungal nail infection. The most commonly used agents are terbinafine, itraconazole, and fluconazole. The medications may cause liver problems or may affect blood cell counts; therefore, blood tests are usually performed before starting therapy and during therapy.
In stubborn fungal nail infections, surgical removal of part of the nail or the entire nail or removing the nail by applying a chemical may be used in addition to topical or oral antifungal agents.
Visit Urgency
See your medical professional if you think you may have nail fungus so they can discuss further treatment approaches and look for possible underlying conditions.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 26th, 2024 at 4:31 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder