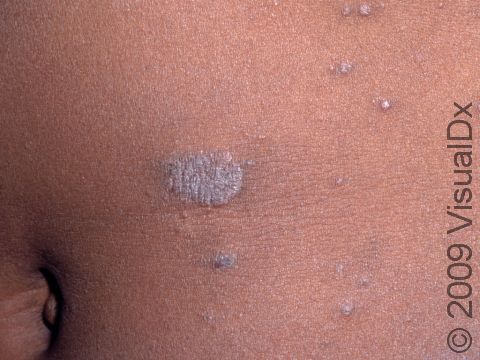
Pityriasis Rosea
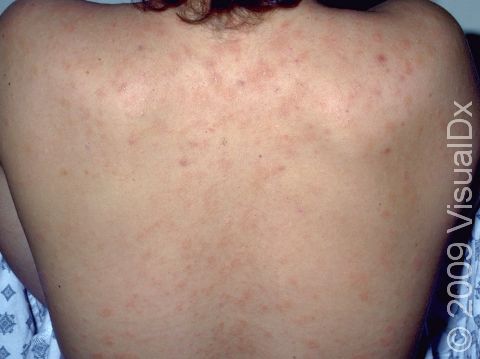
Pityriasis rosea is a common rash that most commonly occurs on the back, chest, and abdomen. It starts fairly quickly, lasts about 6-8 weeks, and is usually not itchy.
The cause of pityriasis rosea is not known, but it may be due to infection with a virus.
Who's At Risk?
Pityriasis rosea can occur in people of any age, race / ethnicity, and sex, but it is most common in older children and young adults (aged 10-40 years). Pityriasis rosea is uncommon in children younger than 5 years.
Signs & Symptoms
The most common locations for pityriasis rosea include the:
- Chest.
- Upper back.
- Neck.
- Abdomen.
- Upper arms.
- Thighs.
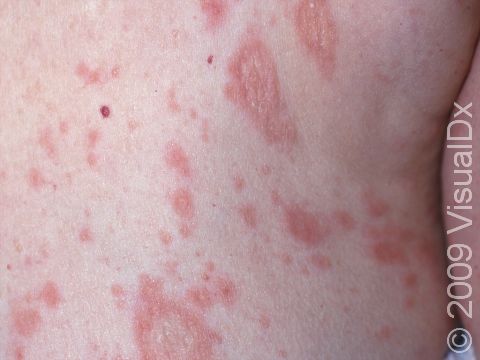
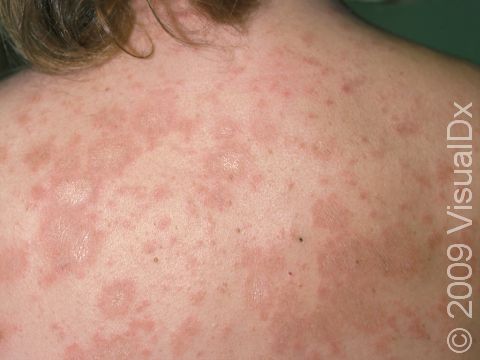
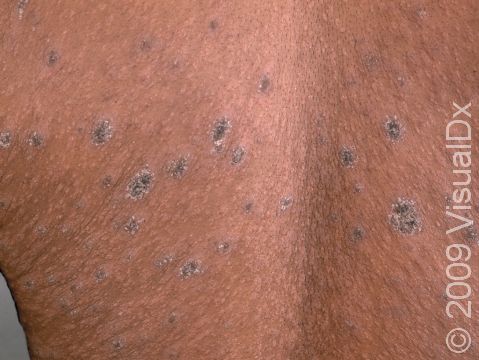
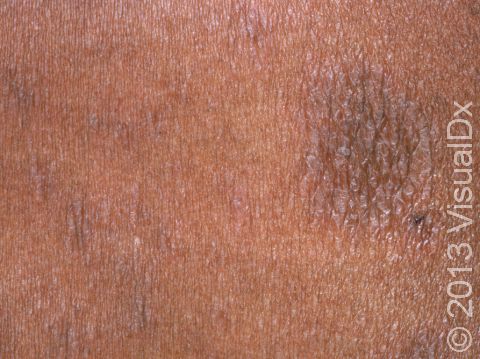
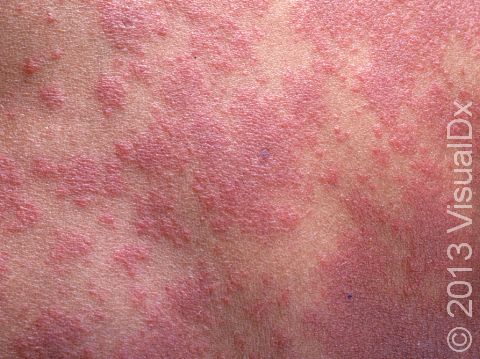
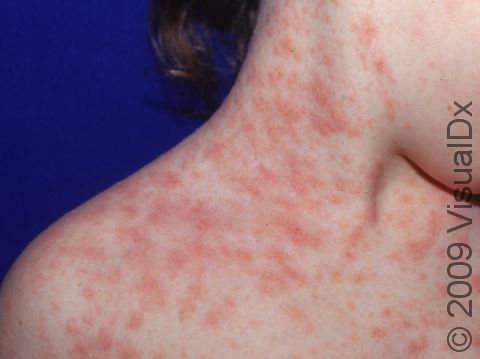
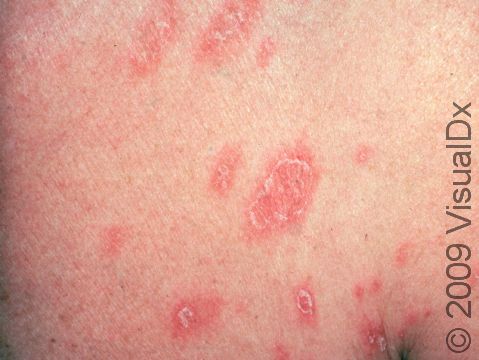
Pityriasis rosea usually begins with a single scaly plaque (a raised area on the skin) ranging from 2-5 cm in size. This first patch is called a “herald patch,” and it is usually located on the trunk, neck, or upper arms. The herald patch is followed 1-3 weeks later by the development of a widespread rash with smaller (0.5-2 cm) oval scaly papules and plaques on the trunk and upper arms. These papules and plaques form a “Christmas tree” pattern on the back. Children sometimes have an unusual form of pityriasis rosea with lesions on the face, wrists, and legs rather than on the trunk. In an uncommon type of pityriasis rosea, the rash may be concentrated in the armpits and groin or on the face, forearms, and shins. In lighter skin colors, the rash can be any shade of pink or red. In darker skin colors, the rash may appear dark red, purple, or darker brown than the normal surrounding skin.
Some children report feeling mildly ill (headache, stuffy nose, muscle aches) for 1-2 weeks before the herald patch forms. Additionally, some children have itching with pityriasis rosea. Becoming overheated by exercising or taking a hot shower may increase itching or make the rash more apparent.
Pityriasis rosea goes away on its own within 6-8 weeks, even without treatment. However, the rash often leaves behind patches of lighter (hypopigmented) or darker (hyperpigmented) skin; these patches are more obvious in darker skin colors and may take months to return to their normal color.
Self-Care Guidelines
The herald patch of pityriasis rosea may be mistaken for ringworm (tinea corporis), but over-the-counter antifungal creams do not improve it. Similarly, the herald patch may look like eczema, but over-the-counter hydrocortisone creams also do not improve it.
Itching with pityriasis rosea can sometimes be reduced by:
- Oatmeal baths.
- Lukewarm (rather than hot) baths and showers.
- Antihistamine pills such as fexofenadine (Allegra), cetirizine (Zyrtec), or loratadine (Claritin) in the daytime and diphenhydramine (Benadryl) at bedtime.
Other than relieving the itch, there are no self-care measures for pityriasis rosea. Although the rash should go away on its own within 6-8 weeks, see a medical professional for evaluation of any widespread rash on your child.
Treatments
In most cases, a medical professional will be able to diagnose the rash by examining your child’s skin. If the rash is atypical, a skin biopsy may be required. These are usually performed by a dermatologist.
In addition, the medical professional may want to do blood tests for other medical conditions.
Because pityriasis rosea goes away on its own, no treatment is required. However, some children with pityriasis rosea have mild-to-severe itching, in which case the clinician may suggest:
- Moisturizing creams or lotions.
- Topical menthol-phenol lotions.
- Prescription topical corticosteroid (cortisone) creams or lotions.
- Oral antihistamine pills.
Visit Urgency
If your child develops a patch of pink, purplish, or brown, scaly skin that does not respond to over-the-counter antifungal cream or hydrocortisone cream, or if your child develops a widespread rash, see their medical professional or a dermatologist for an evaluation.
Be prepared to discuss the following with the medical professional:
- The course of the rash (when it started, whether or not there was a herald patch, etc)
- What treatments, if any, you have tried
- Whether or not any friends or relatives have a similar rash
- Your child’s medication history (making sure you know the names of any medications or supplements your child has taken within the last month)
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 25th, 2024 at 4:24 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder