Hot Tub Rash (Pseudomonas Folliculitis)
Pseudomonas folliculitis, also known as hot tub folliculitis or hot tub rash, is an infection of the hair follicle with Pseudomonas bacteria. It is most commonly seen in people who bathe in a contaminated spa, swimming pool, or hot tub, such as in those with inadequate chlorine levels.
Hot tub rash usually clears up without treatment within 2 weeks.
Who's At Risk?
Hot tub rash can occur in people of any age, race / ethnicity, or sex.
Individuals with hot tub rash usually have a history of one of the following:
- Bathing in a contaminated spa, swimming pool, or hot tub
- Using a contaminated loofah sponge, swimming pool inflatable, or towel
- Wearing a contaminated diving suit
Signs & Symptoms
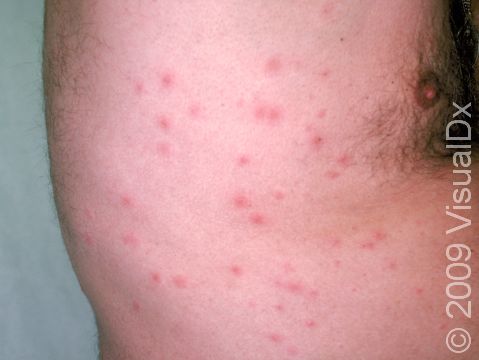
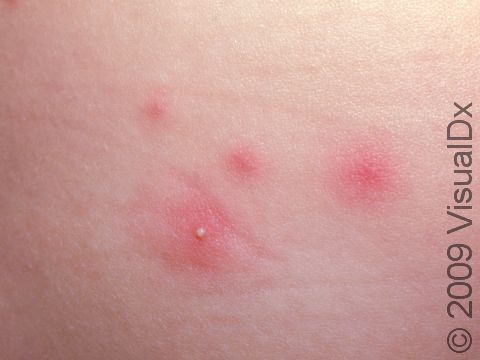
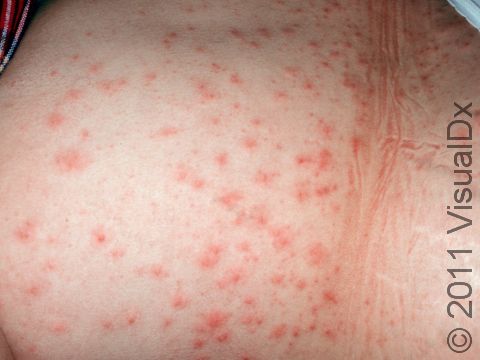
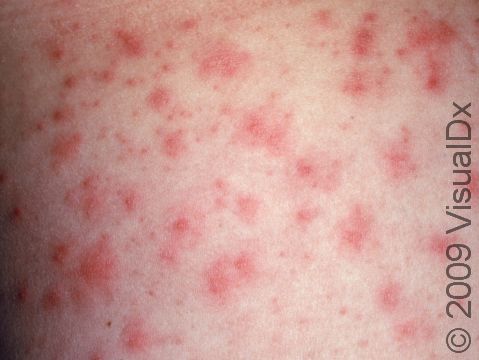
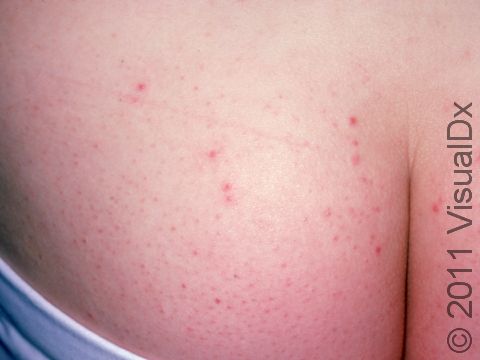
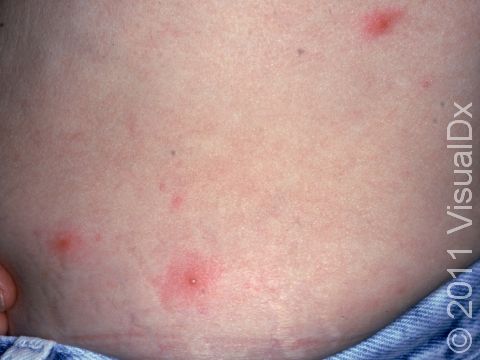
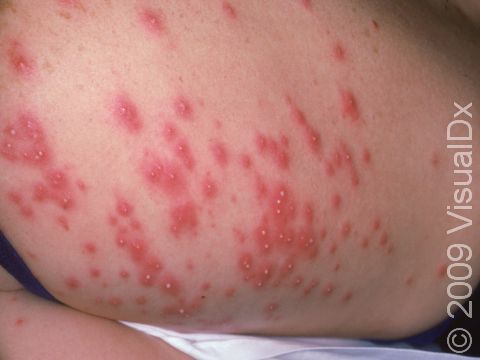
The rash appears as 2-10 mm pink-to-red papules (small, solid bumps) or pustules (pus-filled bumps) that may be covered with scabs. The individual bumps are located around hair follicles and tend to be itchy or tender.
The most common locations for hot tub rash include the:
- “Bathing suit” area (groin and buttocks).
- Trunk.
- Skin folds, such as the underarms.
Hot tub rash typically arises within 1-4 days of exposure to the contaminated water source. In addition to the rash, other symptoms can include mild fever, headache, sore throat, and fatigue. Swollen and tender lymph nodes (glands that help produce antibodies, special proteins that fight off infection) may occur. Breast tenderness occasionally develops in both men and women, as glands in the nipple may become infected.
Although hot tub rash usually resolves within 7-14 days without treatment, the rash may leave behind patches of darker (hyperpigmented) skin. These patches are more pronounced in people with darker skin colors and may take months to return to normal pigmentation.
Self-Care Guidelines
If the rash is itchy, taking an over-the-counter antihistamine (eg, Zyrtec, Benadryl) may be helpful.
To prevent hot tub rash in the future, proper maintenance and chlorination of pools, spas, and hot tubs is essential. Sponges and loofahs should be completely dried between uses to kill any bacteria.
Treatments
Your medical professional may want to obtain a bacterial culture of one of the pus-filled bumps to establish the diagnosis.
No special therapy is required, typically, as the rash should go away on its own. However, in severe cases, your medical professional may recommend:
- Acetic acid compresses.
- An oral antibiotic, such as ciprofloxacin.
- Topical antibiotic cream, such as gentamicin.
Visit Urgency
Make an appointment with your medical professional if you develop an itchy or tender rash, especially if it is associated with fever, swollen lymph nodes, or breast tenderness.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 17th, 2024 at 2:31 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder