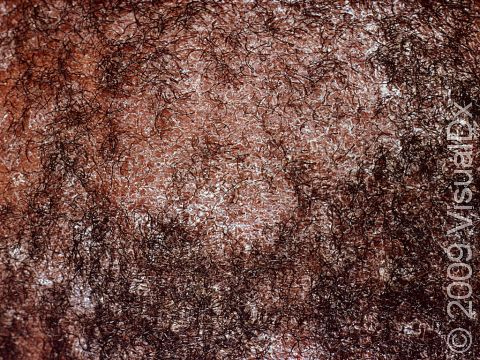Scalp Ringworm (Tinea Capitis)
Tinea capitis is the medical term for ringworm, a type of fungal infection, of the scalp. The rash forms a scaly, round plaque (a raised area of skin larger than a thumbnail) that sometimes clears or improves in the middle, making it look like a ring. Ringworm is contagious and is acquired by contact with infected people, animals, or objects (such as towels, combs, and pillows). Scalp ringworm should be treated by prescription medicine because if left untreated, the affected area can develop hair loss (alopecia) and sometimes another more serious infection called a kerion.
Who's At Risk?
Anyone can get scalp ringworm, but it is most commonly seen in children younger than age 10 years.
In adults, scalp ringworm is most common in those who are in contact with animals (as the fungal infection can be passed from animals to humans) and in those who have a suppressed immune system.
Signs & Symptoms
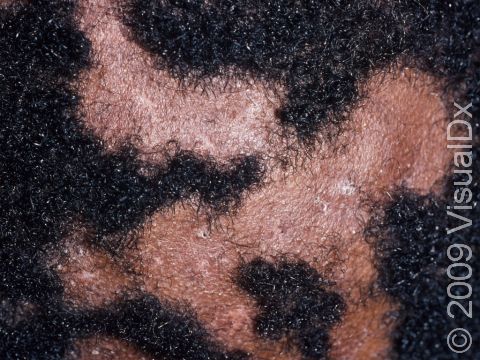
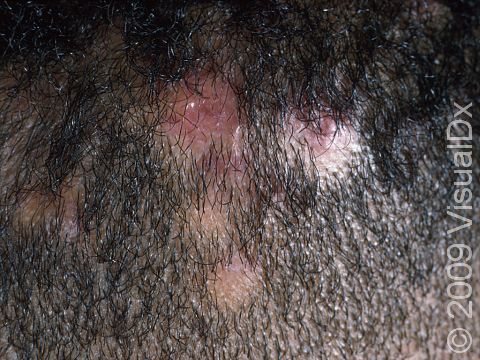
Scalp ringworm appears as one or more round or oval plaques covered with gray scale, and there is often hair loss in the area. In lighter skin colors, the border can be pink or red, whereas in darker skin colors, it can be dark red, purple, brown, or grayish. The area may be inflamed, and small pustules (pus-filled bumps) may sometimes be seen. There may be tiny black dots on the surface of the scalp from broken hairs.
Although the scalp is the most common location for this type of ringworm, the eyebrows and eyelash areas are also occasionally affected.
The lymph nodes at the back of the scalp, behind the ears, or along the sides of the neck may be swollen. Scalp ringworm is usually itchy.
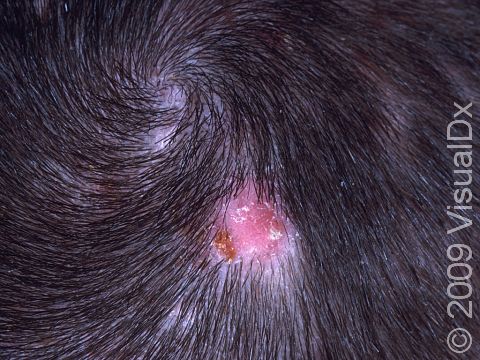
One complication of scalp ringworm is a kerion, a thick, “boggy” or “mushy” nodule (a solid-raised bump that is firm to the touch) or plaque (a raised or bumpy area larger than a thumbnail) on the skin. If not treated aggressively, a kerion can lead to scarring and permanent hair loss.
Self-Care Guidelines
There are no effective self-care measures to treat scalp ringworm.
In order to prevent scalp ringworm, be sure to avoid close contact with infected people and pets.
If you have scalp ringworm, because it is very contagious, avoid contact sports until lesions have been treated for at least 48 hours. Do not share towels, clothing, or other personal items with others until the lesions have cleared.
Treatments
To confirm the diagnosis of scalp ringworm, your medical professional may scrape some scales onto a slide and examine it under a microscope. This procedure, called a KOH (potassium hydroxide) preparation, allows the medical professional to look for signs of a fungal infection.
The medical professional may also perform a skin culture to document the presence of fungus or to discover the particular organism that is causing the scalp ringworm.
Scalp ringworm is treated with oral antifungal medicines because the fungus invades deep into the hair follicle, where topical creams and lotions cannot penetrate. Scalp ringworm usually requires at least 6-8 weeks of treatment with oral antifungal pills, such as with:
- Terbinafine.
- Fluconazole.
- Itraconazole.
- Griseofulvin.
The medical professional may also prescribe a medicated shampoo to reduce the risk of spreading the infection to others, such as:
- Selenium sulfide shampoo.
- Ketoconazole shampoo.
Visit Urgency
If you have hair loss or itchy, scaly patches on the scalp, especially if the affected areas are deep and tender or if you have a fever or swollen lymph glands, see a medical professional.
Have any household pets or farm animals evaluated by a veterinarian to make sure they do not have a fungal infection. If the veterinarian discovers an infection, be sure to have the animal(s) treated.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 17th, 2024 at 4:34 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder