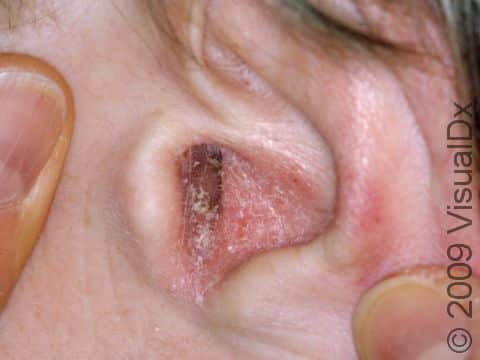
Seborrheic Dermatitis
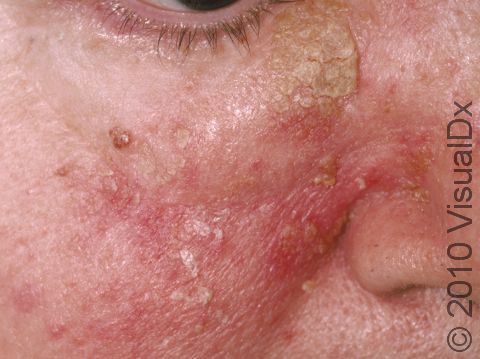
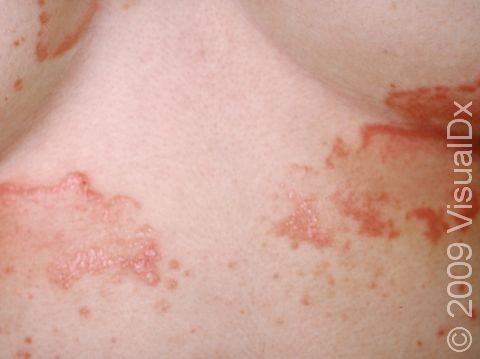
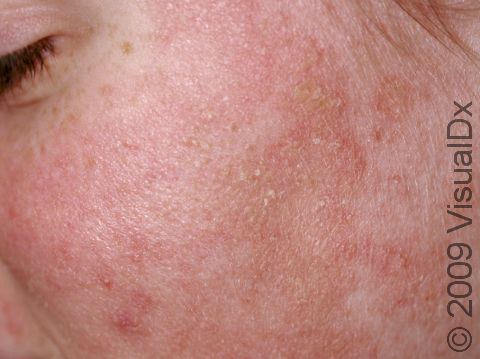
Seborrheic dermatitis, also known as seborrhea, is a common noncontagious condition of skin areas rich in oil glands (the face, scalp, and upper trunk). Seborrheic dermatitis causes overproduction and flaking of skin cells and sometimes itchy skin. It can vary in severity from mild dandruff of the scalp to scaly patches on the skin. Normal skin yeast called Pityrosporum ovale lives in oil-rich skin regions and plays a role in this disorder; the changes seen in the skin are due to the body’s inflammatory response to the yeast on the skin. Seborrheic dermatitis seems to worsen with stress, dry weather, and infrequent shampooing. Although there is no cure for seborrheic dermatitis, control is usually possible with medicated shampoos and topical steroids (when inflammation is prominent).
Who's At Risk?
Dandruff occurs in 15%-20% of the population, and more severe seborrheic dermatitis (with flaking and inflamed skin) occurs in 3%-5% of all people. Seborrheic dermatitis affects all races / ethnicities and may be a bit worse in men. It typically starts after puberty (although babies may have a variant called cradle cap). The severity of seborrheic dermatitis peaks around age 40 and then may improve. Severe seborrheic dermatitis is frequently seen in people with Parkinson disease, central nervous system problems, and HIV infection.
Signs & Symptoms
- The scalp is itchy and sheds white, oily skin flakes.
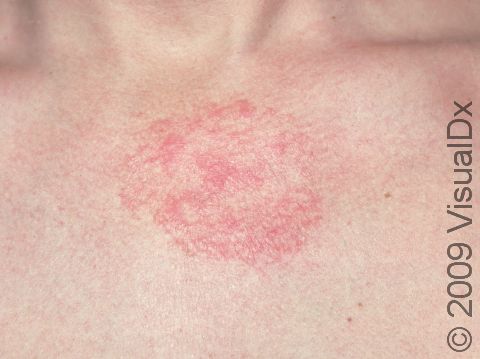
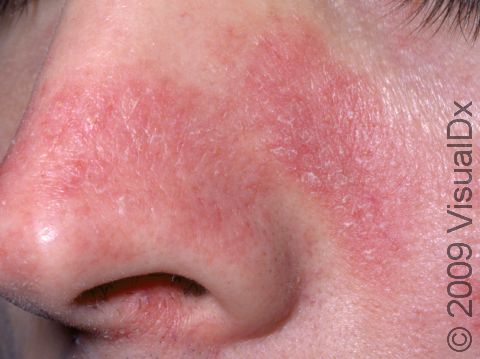
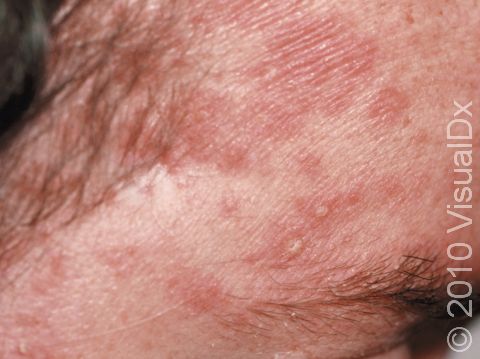
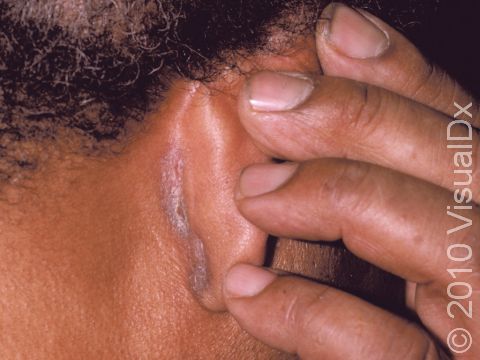
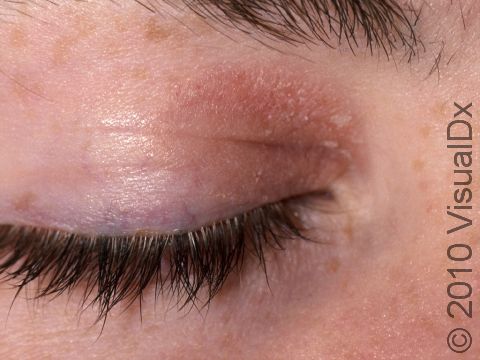
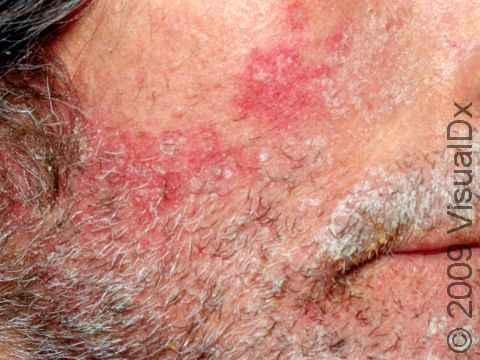
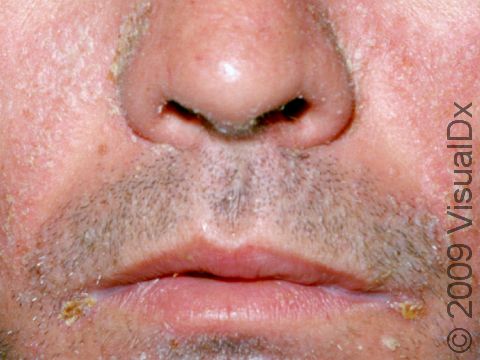
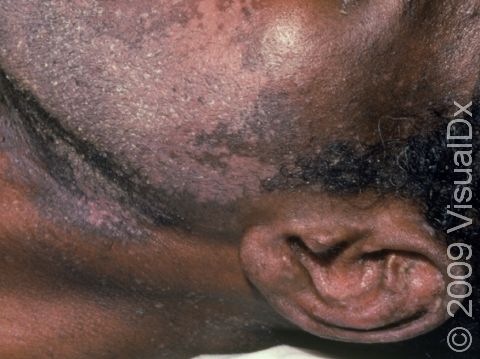
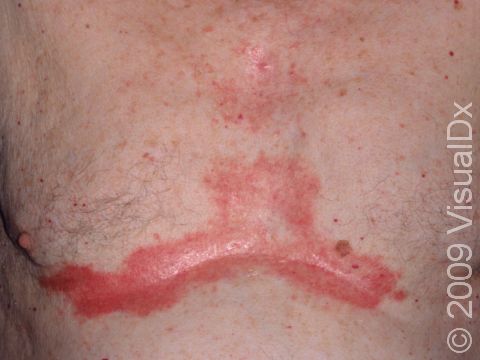
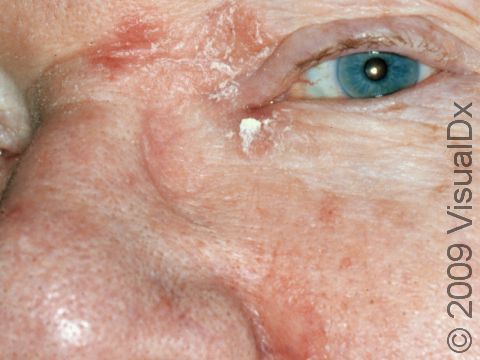
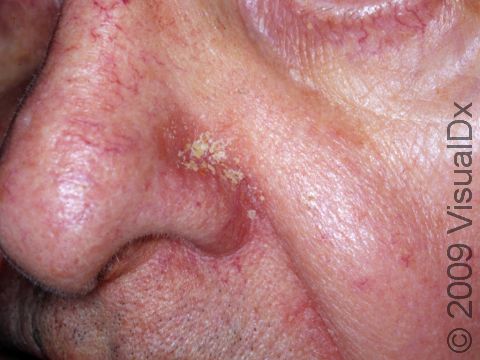
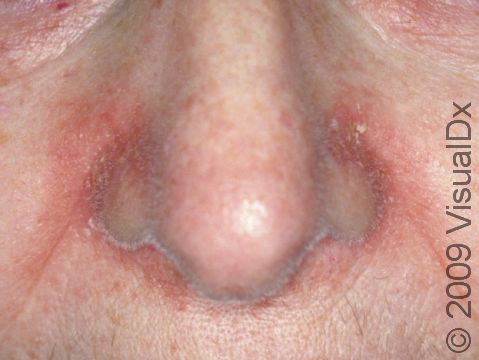
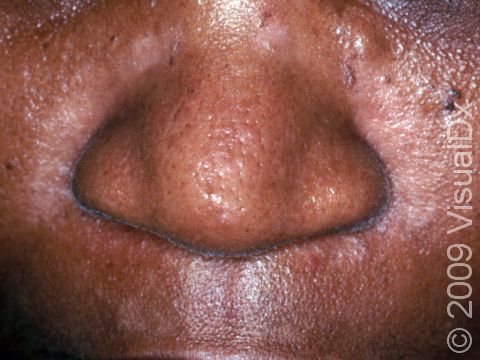
- One or more of the following areas has patches of scaly skin: the scalp, hairline, forehead, eyebrows, in between the eyebrows, the area of the eyelid between the eye and the eye lashes (the free lid margin), creases of the nose and ears, ear canals, beard area, breastbone, midback, groin, and underarms. In lighter skin colors, affected areas may appear pink or red; in darker skin colors, the redness may be subtle, or affected areas may appear purplish or darker brown, but the affected areas may also look lighter in color (hypopigmented).
Seborrheic dermatitis may be:
- Mild – only some flaking and skin color change (as outlined above) in a few small areas.
- Moderate – several areas affected with bothersome skin color change and itch.
- Severe – large areas of skin color change and severe itch that do not improve with self-care measures.
Self-Care Guidelines
Most cases of seborrheic dermatitis are easy to control with nonprescription home treatments. These include:
- Frequent shampooing or a longer lather time with shampoo. If a regular daily shampoo fails, consider an over-the-counter dandruff shampoo. There are several types on the market, and one may work better for one individual than another.
- Shampoos containing ketoconazole (Nizoral), selenium sulfide (Selsun Blue), 2% pyrithione zinc (Head & Shoulders), salicylic acid (Neutrogena T/Sal), or tar-based (Neutrogena T/Gel) compounds may be helpful. Consider occasionally rotating shampoos because the ability of how well a product works (its efficacy) can change with time.
- If the scalp is covered with widespread, dense scale, the scale may first be removed by applying warm mineral oil or olive oil to the scalp and washing several hours later with a detergent, such as a dishwashing liquid or a tar shampoo.
- Some over-the-counter creams will help if the medicated shampoo is not working well enough. These can be added to the shampoo until there is improvement and then can be discontinued; these creams can be used again temporarily as needed and include:
- Creams that reduce the Pityrosporum yeast (clotrimazole [Lotrimin], miconazole [Monistat]).
- Hydrocortisone (eg, Cortaid) cream, which may work well at first but may be less helpful if used for a long time.
- Managing eyelid inflammation (called blepharitis) by gentle cleaning of the skin around the eyelashes (eyelid margins) with a cotton swab and baby shampoo (eg, Johnson’s Baby Shampoo).
Treatments
- Corticosteroid creams, lotions, or solutions
- Sulfur or sulfacetamide products, such as a wash, cream, or lotion, applied on the skin (topically)
- Prescription-strength ketoconazole shampoo or cream
- Tacrolimus (Protopic) ointment or pimecrolimus (Elidel) cream
- Roflumilast foam (Zoryve)
Visit Urgency
Seek medical help from a dermatologist or other medical professional if there is no response to self-care measures.
Trusted Links
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Last modified on February 25th, 2026 at 1:27 pm

Not sure what to look for?
Try our new Rash and Skin Condition Finder