Tinea Versicolor
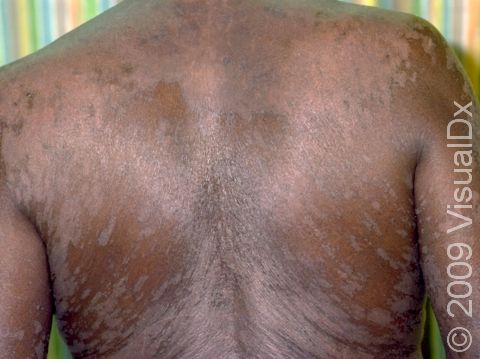
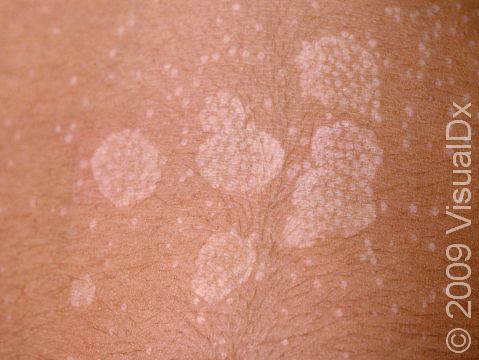
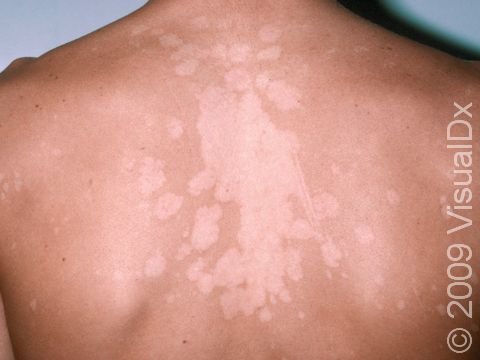
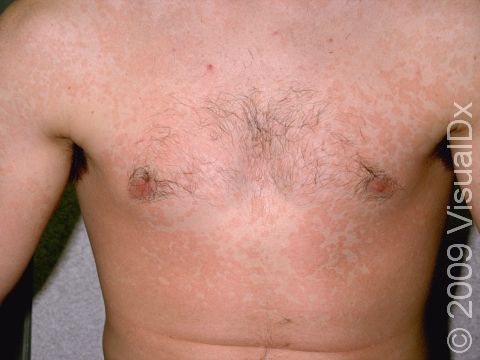
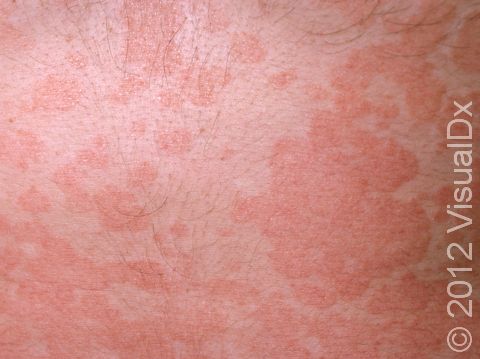
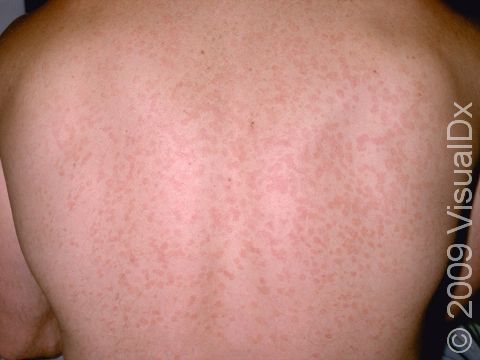
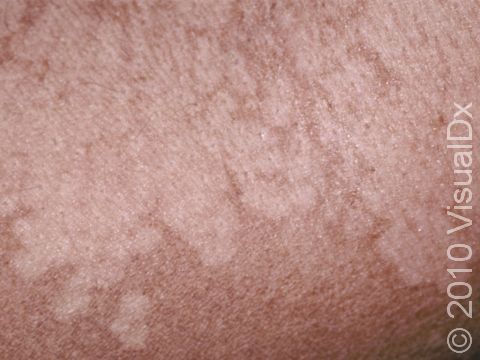
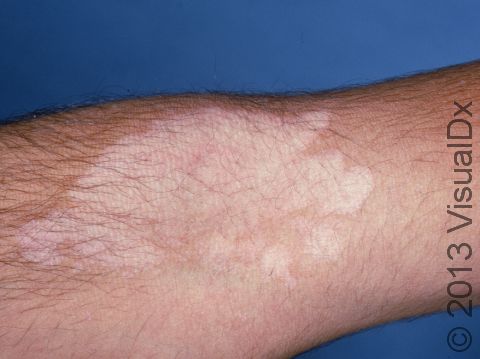
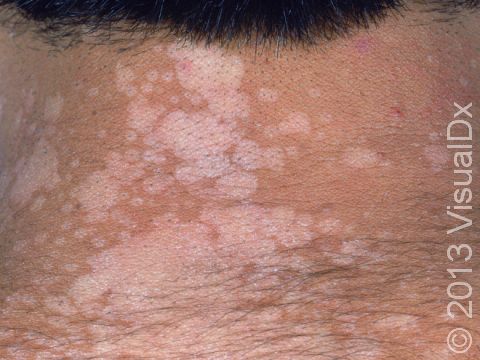
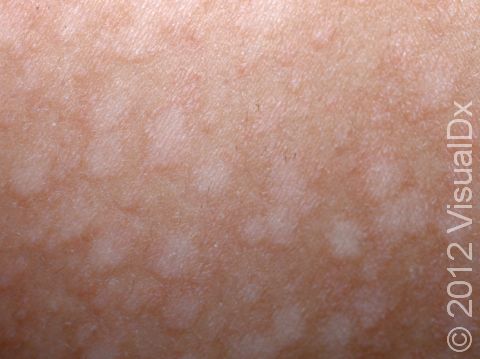
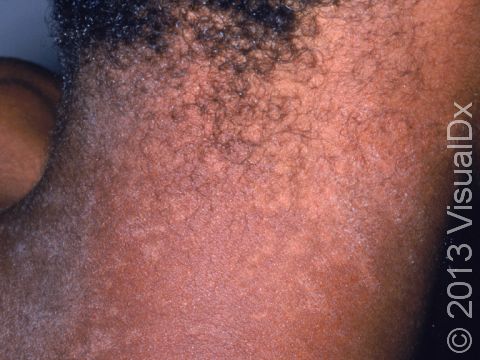
Tinea versicolor, also known as pityriasis versicolor, is a common skin condition caused by a surface (superficial) infection with a yeast called Malassezia that commonly lives on the skin. Under certain conditions, such as warm, oily, and moist skin, the yeast can overgrow and cause a rash that may appear as tan, pink, brown, or white patches (flat areas that are larger than a thumbnail) with a layer of fine scale. In some people, the patches are darker than their usual skin color (hyperpigmented). In others, the patches may be lighter (hypopigmented). Sometimes the patches may be both lighter and darker in different areas. In darker skin colors, the rash is most often lighter than the surrounding skin. Although it is an infection, tinea versicolor is not contagious.
Who's At Risk?
Tinea versicolor can develop in people starting in adolescence through adulthood. It can affect people of any race or sex.
Tinea versicolor most commonly affects people living in tropical areas with high humidity and high temperatures. In milder climates, teens and young adults are affected most frequently. Tinea versicolor is uncommon in young children or in adults older than 65.
Some conditions make tinea versicolor more likely to occur:
- Living in a warm, humid climate
- Having oily skin
- Being pregnant
- Sweating frequently or excessively
Signs & Symptoms
The most common locations for tinea versicolor include the:
- Chest and upper back.
- Upper arms.
- Abdomen.
- Neck.
- Thighs.
Tinea versicolor appears as many white, pink, salmon-colored, tan, or brown patches ranging in size from 1 to 3 cm. The individual lesions can join together to form large patches. Most lesions have a very fine, flaky surface (scale).
The yeast that causes the condition produces a substance that can temporarily bleach the underlying skin to a lighter color. Even after the infection has cleared, the spots may be hypopigmented patches that may not get their normal color back for many months. These hypopigmented spots do not tan normally. The lighter areas are more obvious in darker skin colors.
Even if the color has not returned to normal after treatment, the flakiness of the skin should have resolved.
Tinea versicolor does not usually cause any symptoms, but some people report minor itching, especially when they get sweaty.
Self-Care Guidelines
If you suspect you have tinea versicolor, you can try an over-the-counter antifungal cream such as clotrimazole (Lotrimin) or miconazole (Monistat). Over-the-counter shampoos such as those containing selenium sulfide (Selsun Blue), ketoconazole (Nizoral), or zinc pyrithione (Head & Shoulders) can be applied as a body wash to the affected areas in the shower and then rinsed off well. However, if the condition does not seem to be getting better after 2 weeks of daily treatment, see a dermatologist or another medical professional for evaluation.
If you have been treated for tinea versicolor, avoid wearing tight-fitting clothing. Also, sun exposure may make the remaining light-colored areas more apparent, so avoid sun exposure or wear sunscreen until the spots have returned to their normal color.
Treatments
To confirm the diagnosis, your medical professional may scrape some of the surface flakes onto a glass slide and examine them under a microscope. This procedure, called a KOH (potassium hydroxide) preparation, allows for identification of the yeast that causes the infection.
Once a diagnosis of tinea versicolor has been confirmed, the medical professional may recommend one of the following treatments:
- Over-the-counter selenium sulfide, ketoconazole, or zinc pyrithione shampoo, if these have not yet been tried
- Prescription-strength ketoconazole shampoo
- Antifungal cream such as ketoconazole (Extina, Ketozole), econazole (Ecoza), or ciclopirox (Loprox)
- Antifungal pills such as fluconazole (Diflucan) or itraconazole (Sporanox)
Recurrence of the infection after treatment is common. Your medical professional may recommend a preventive or maintenance treatment to use during the warmer, more humid months, such as an antifungal cream or shampoo applied every week.
Visit Urgency
If these self-care measures do not work or if your rash is spreading, see your medical professional.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 13th, 2024 at 10:58 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder