Cellulitis
Cellulitis is an infection of the skin that is most often caused by the bacteria Staphylococcus (“staph”) and Streptococcus (“strep”). These bacteria are able to enter the skin through small cracks (fissures), causing sudden redness, swelling, and warmth in an area of the skin. Cellulitis is sometimes accompanied by fever, chills, and feeling fatigued.
If the infection is left untreated for too long, cellulitis can result in abscesses (swollen, warm, tender lumps filled with pus) or the spread of bacteria into the bloodstream (bacteremia). However, most cases of cellulitis resolve with appropriate antibiotic therapy.
Who's At Risk?
Cellulitis can occur in anyone or any age, race / ethnicity, and sex. Factors that increase the risk of developing cellulitis include:
- Diabetes.
- Lymphedema.
- Skin wounds.
- Chronic lower leg swelling (edema).
- Athlete’s foot (tinea pedis).
- Bites from insects, animals, or other humans.
- Obesity.
- Weakened immune system due to underlying illness or medication.
Signs & Symptoms
Cellulitis can affect any part of the body, but the most common locations are the:
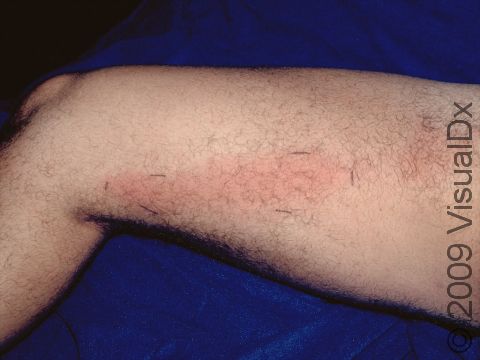
- Lower legs.
- Arms or hands.
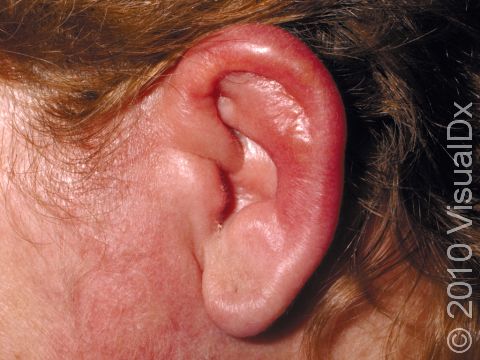
- Face.
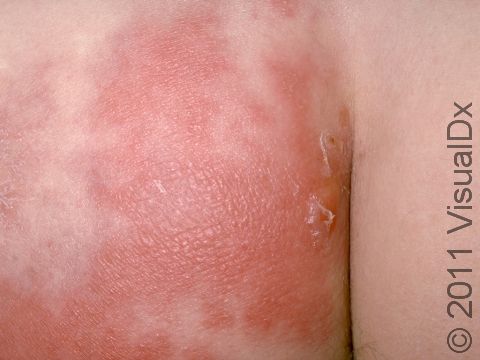
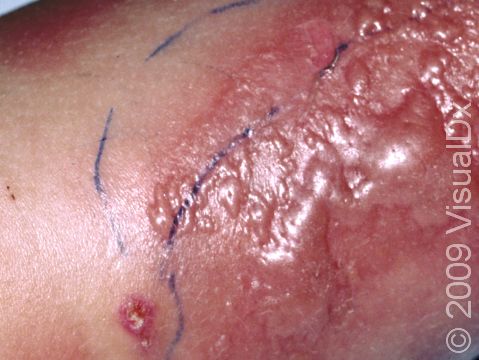
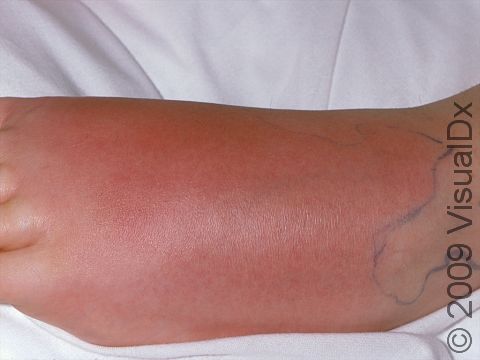
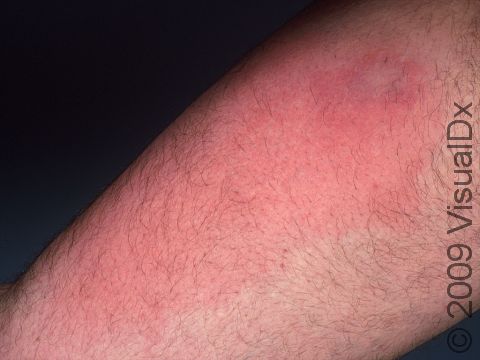
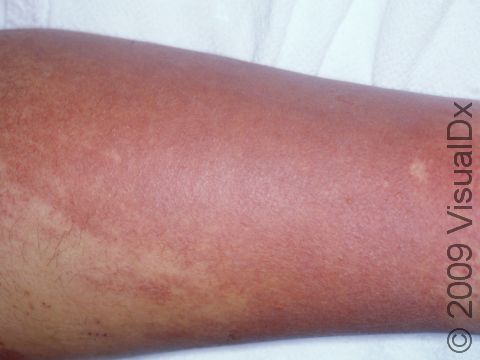
Cellulitis often appears initially as minimally inflamed skin. The involved area may rapidly become swollen, warm, and tender to the touch and increase in size as the infection spreads. In lighter skin colors, the area may be any shade of pink or red. In darker skin colors, the redness may be harder to see, or it may appear more purple or dark brown. Occasionally, red streaks may radiate outward from the cellulitis. Vesicles (small blisters) or bullae (pus-filled lesions larger than a thumbnail) may also be present.
Cellulitis may be accompanied by swollen lymph nodes, fever, chills, and fatigue.
Self-Care Guidelines
If you think you have cellulitis, make an appointment to see your medical professional. While you are waiting for the appointment, elevating the involved body part, if you are able, can help decrease swelling. A cool, clean, moist towel can be applied to the area to decrease pain.
Treatments
Your medical professional will usually be able to easily diagnose cellulitis by examining the affected area. Sometimes they may want to get additional information by ordering blood tests and/or performing a bacterial culture to identify the specific bacterium that is causing the cellulitis as well as to test its susceptibility to different antibiotics, which helps guide treatment decisions.
While waiting for the results from the bacterial culture, your medical professional may want to start you on an antibiotic to fight the most common bacteria that cause cellulitis. Once the final culture results have returned, your medical professional may change the antibiotic you are taking, especially if your infection is not improving.
Mild cases of cellulitis in a healthy person can be treated with oral antibiotics. Common antibiotics that are used to treat cellulitis include:
- Trimethoprim-sulfamethoxazole (eg, Bactrim).
- Doxycycline (eg, Vibramycin).
- Minocycline (eg, CoreMino).
- Clindamycin (eg, Cleocin).
- Dicloxacillin.
- Cephalexin (eg, Keflex).
- Linezolid (eg, Zyvox).
If you are very sick or have other chronic illnesses that may complicate your recovery, you may need to be hospitalized to receive intravenous antibiotics. Common intravenous antibiotics that are used to treat cellulitis include:
- Vancomycin (eg, Firvanq, Vancocin).
- Linezolid.
- Cefazolin (eg, Claforan).
- Oxacillin.
- Nafcillin.
- Clindamycin.
If your medical professional prescribes antibiotics, be sure to take the full course of treatment. In addition to prescribing antibiotics, they will likely want to make sure that your underlying medical problems, if any, are being adequately managed.
Visit Urgency
If you develop a painful, warm, enlarging area on your skin that is red or a darker color than your surrounding skin, make an appointment with your medical professional as soon as possible to get treatment and to avoid complications that may occur if cellulitis is left untreated. If you also have fever and chills or if the area involves the face, you should go to urgent care or the emergency room.
If you are currently being treated for a skin infection that has not improved after 2-3 days of antibiotics, return to your medical professional. You may need treatment with different medications, or the infection may have spread deeper into your skin.
References
Bolognia J, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018.
James WD, Elston D, Treat JR, Rosenbach MA. Andrew’s Diseases of the Skin. 13th ed. Philadelphia, PA: Elsevier; 2019.
Kang S, Amagai M, Bruckner AL, et al. Fitzpatrick’s Dermatology. 9th ed. New York, NY: McGraw-Hill Education; 2019.
Paller A, Mancini A. Paller and Mancini: Hurwitz Clinical Pediatric Dermatology. 6th ed. St. Louis, MO: Elsevier; 2022.
Last modified on June 14th, 2024 at 10:34 am

Not sure what to look for?
Try our new Rash and Skin Condition Finder